“Why Do I Still Get Rosacea Breakouts and Dark Spots Even When I’m Using My Cream?”
A 40-year-old patient in Katy, TX experienced persistent rosacea flares and dark spots despite treatment. Learn how dermatologists manage rosacea and prevent hyperpigmentation.
By: Dr. Caroline Vaughn
A Real Patient Case from Village Dermatology in Katy & Houston, Texas
Rosacea is one of the most common—and frustrating—chronic skin conditions we treat. Many patients feel discouraged when they are already using prescription creams but still experience flare-ups and lingering dark spots.
This case highlights a 40-year-old female dealing with persistent rosacea flares and post-inflammatory hyperpigmentation (PIH) despite appropriate topical therapy.
Patient Case Overview
The patient returned for follow-up after starting a triple rosacea cream (azelaic acid, metronidazole, and ivermectin).
She reported:
Improvement overall with her prescription cream
Continued intermittent inflammatory bumps
Concern about dark spots (PIH) after flares
On exam:
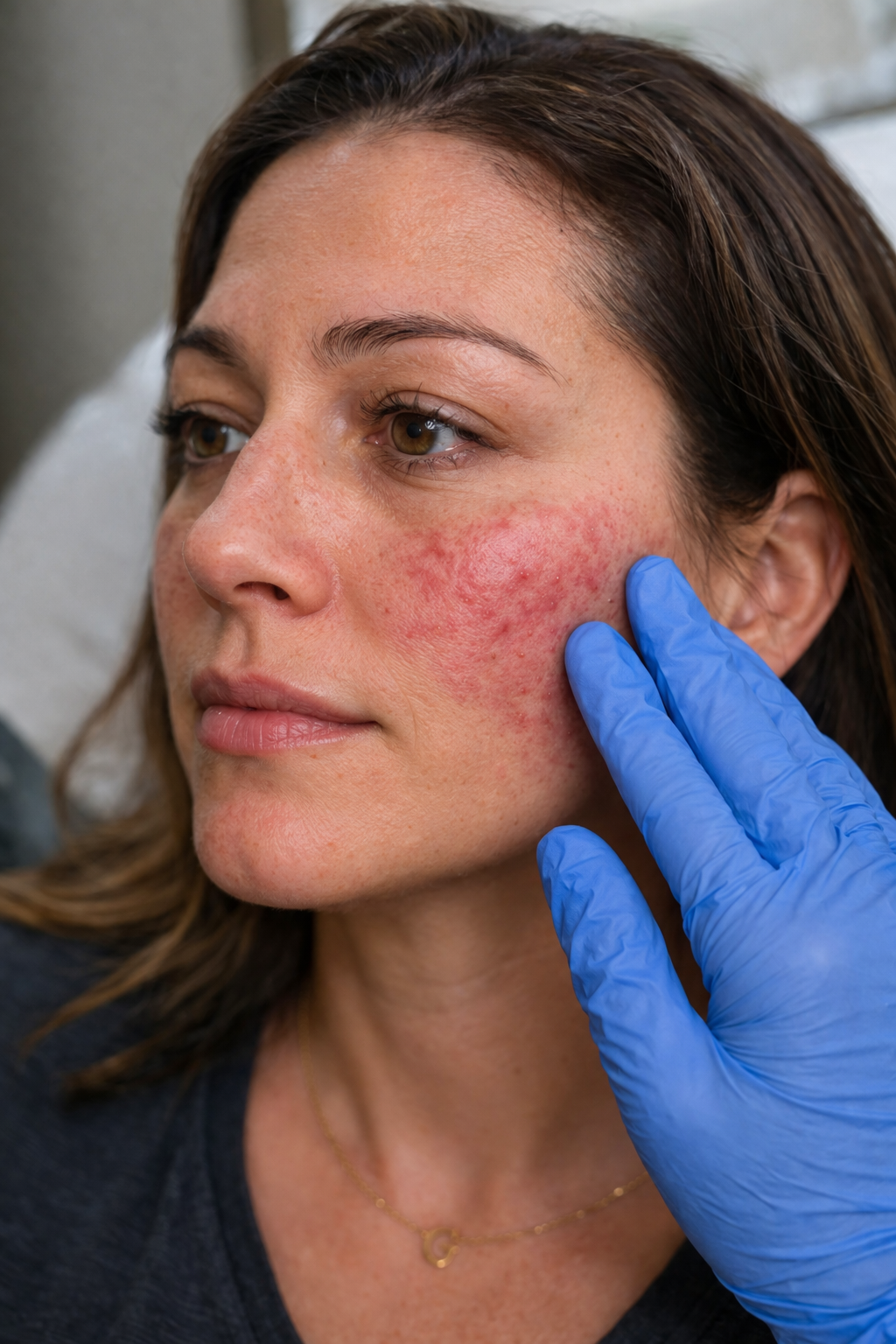
Mild inflammatory papules on the cheeks
Classic malar distribution of rosacea
Understanding Rosacea
Rosacea is a chronic inflammatory skin condition that primarily affects the central face.
Common symptoms:
Persistent redness
Acne-like bumps
Flushing and sensitivity
Visible blood vessels
Rosacea tends to flare and calm repeatedly, rather than fully resolve.
Why Am I Still Breaking Out?
This is one of the most common patient questions.
Even with good topical therapy:
Rosacea is chronic, not curable
Topicals may not fully control deeper inflammation
Triggers like heat, stress, alcohol, and spicy foods can still cause flares
In this case, the patient’s cream helped—but wasn’t enough to fully suppress inflammation.
What About the Dark Spots (PIH)?
Post-inflammatory hyperpigmentation (PIH) can occur after rosacea flares.
Important points:
PIH develops after inflammation heals
Treating PIH aggressively can irritate skin and worsen rosacea
The best strategy is preventing flares first
That’s why we focused on better inflammation control before targeting pigmentation.
Updated Treatment Plan
To improve long-term control, we adjusted her regimen:
Oral Anti-Inflammatory Therapy
Helps reduce inflammation without acting as a traditional antibiotic
Sulfur-Based Cleanser
Helps reduce bacteria and inflammation
Particularly effective for rosacea-prone skin
Continue Triple Cream
Azelaic acid
Metronidazole
Ivermectin
Essential Skin Care Tips for Rosacea
We reinforced gentle, consistent skincare:
Choose gentle cleansers and moisturizers
Green-tinted moisturizers can help reduce visible redness
Avoid harsh exfoliants or irritating products
Common Rosacea Triggers to Avoid
Patients should monitor and minimize:
Sun exposure
Heat and hot showers
Alcohol
Spicy foods
Stress
When Should You Follow Up?
You should return if:
Flares continue despite treatment
Symptoms worsen
You develop deeper nodules or cysts
In this case, follow-up was scheduled in 4–5 months to assess improvement.
Expert Rosacea Care in Katy & Houston, TX
Village Dermatology specializes in managing chronic rosacea and sensitive skin conditions, helping patients across Katy and Houston, Texas achieve clearer, calmer skin with:
Customized combination therapies
Medical and cosmetic treatment options
Long-term skin health strategies
“Why Does My Hand Rash Keep Coming Back Even After Treatment?”
A 52-year-old patient in Katy, TX struggled with a recurring hand rash initially thought to be psoriasis. Learn how contact dermatitis is diagnosed and treated effectively.
By: Dr. Caroline Vaughn
A Real Patient Case from Village Dermatology in Katy & Houston, Texas
Chronic hand rashes can be frustrating—especially when they seem to improve, only to flare up again weeks later. At Village Dermatology, we frequently evaluate patients with persistent hand dermatitis, which is often mistaken for other skin conditions like psoriasis.
This case highlights a 52-year-old male with a recurring rash on his fingers that required careful diagnosis and targeted treatment.
Patient Case Overview
The patient presented with:
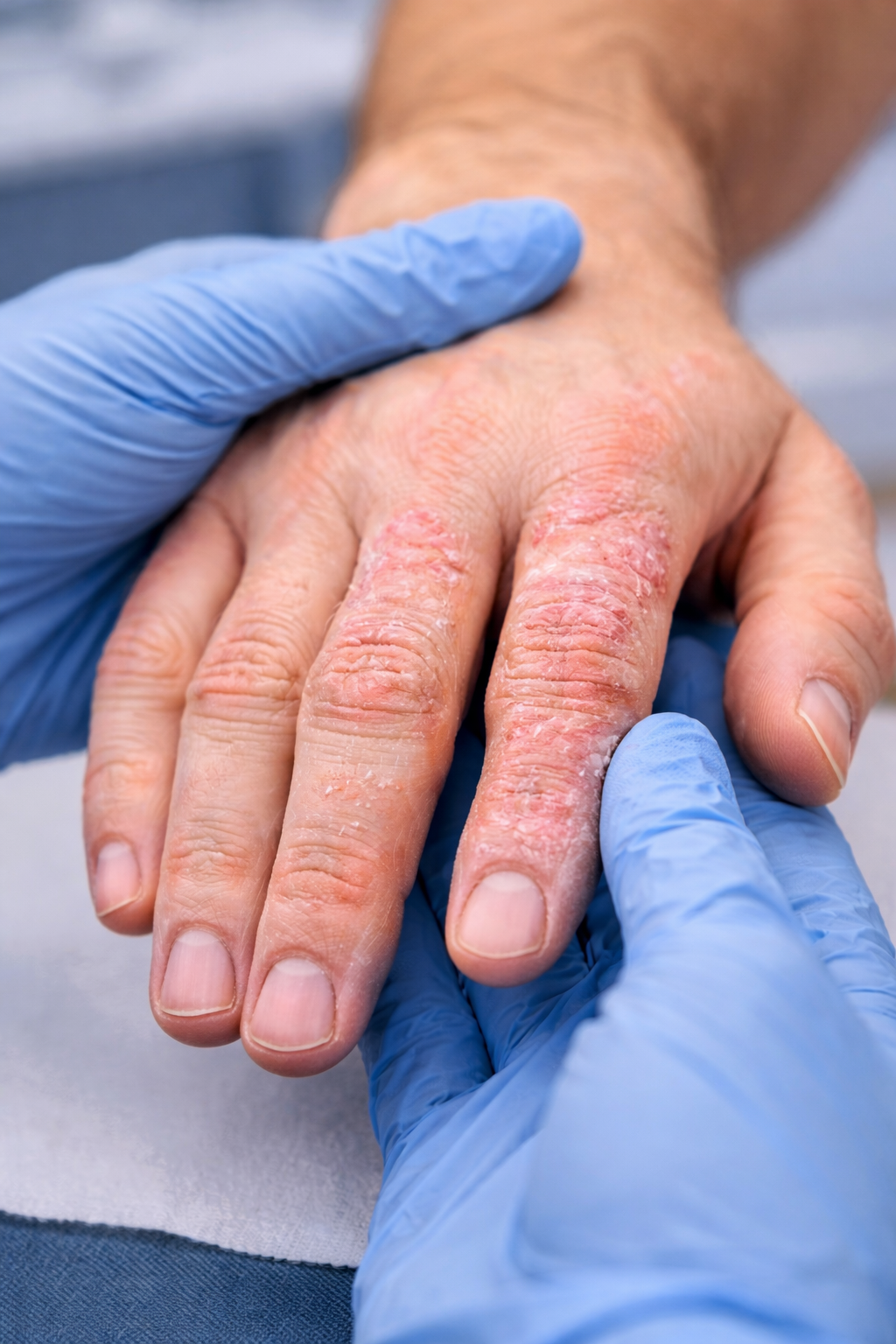
Itchy, moderate rash on the fingers
Involvement of the right index and middle fingers and left index finger
Symptoms recurring intermittently since 2020
Relevant History:
Previously diagnosed with dyshidrotic eczema
Later told it could be psoriasis, but treatment was inconsistent
Rash resolved temporarily, then returned after about 6 weeks
Recently prescribed clobetasol (high-potency topical steroid)
Final Diagnosis: Contact Dermatitis
After a detailed evaluation, the presentation was more consistent with contact dermatitis, rather than psoriasis.
Why psoriasis was less likely:
Limited to only a few fingers
No nail involvement
No joint pain (rules against psoriatic arthritis)
No widespread plaques elsewhere on the body
This pattern strongly suggests external irritation or allergic exposure as the root cause.
What Is Contact Dermatitis?
Contact dermatitis is a skin reaction caused by exposure to irritants or allergens.
Common triggers include:
Soaps and cleansers
Fragrances and skincare products
Metals (nickel)
Occupational exposures (chemicals, gloves, water)
Symptoms:
Red, itchy rash
Dry, cracked skin
Burning or irritation
Why Does It Keep Coming Back?
Many patients ask this exact question.
The answer: ongoing exposure to triggers
Even with treatment:
If the irritant isn’t removed, the rash will return
Some products labeled “moisturizing” can actually worsen irritation
Frequent handwashing can damage the skin barrier
In this case, certain skincare products were likely contributing to recurrence.
Treatment Plan and Recommendations
Topical Steroid Therapy
Continue clobetasol 0.05% as prescribed
Helps reduce inflammation and itching
Moisturizer Optimization
Switch to fragrance-free, hypoallergenic options:
Eucerin
Neutrogena Norwegian Formula
Continue O’Keeffe’s as needed
Discontinue potential irritants like certain scented products
Skin Care Routine
Use Dove sensitive skin soap
Avoid harsh soaps like Dial
Apply moisturizer after every hand wash
Apply steroid after shower and once more during the day
Overnight Repair
Apply Vaseline with cotton gloves overnight to restore skin barrier
When Is Patch Testing Needed?
If symptoms persist, patch testing may be recommended to identify specific allergens causing the reaction.
When Should You See a Dermatologist?
You should seek care if:
Rash lasts more than a few weeks
Symptoms keep recurring
Over-the-counter treatments are ineffective
Skin becomes cracked, painful, or infected
Expert Hand Dermatitis Treatment in Katy & Houston, TX
Village Dermatology provides expert care for chronic rashes and hand dermatitis, helping patients across Katy and Houston, Texas identify triggers and achieve long-term relief through personalized treatment plans.
“Why Is My Psoriasis Getting Worse Even After Trying Biologic Treatment?”
A 35-year-old patient in Katy, TX experienced worsening psoriasis despite prior biologic therapy. Learn how advanced treatments like Skyrizi can help manage severe psoriasis.
By: Dr. Ashley Baldree
A Real Patient Case from Village Dermatology in Katy & Houston, Texas
Psoriasis can be frustrating—especially when it flares despite prior advanced treatments. At Village Dermatology, we often help patients navigate moderate-to-severe psoriasis when standard therapies are no longer effective.
This case highlights a 35-year-old male with widespread psoriasis who previously failed biologic therapy and required a more advanced treatment approach.
Patient Case Overview
The patient presented with:
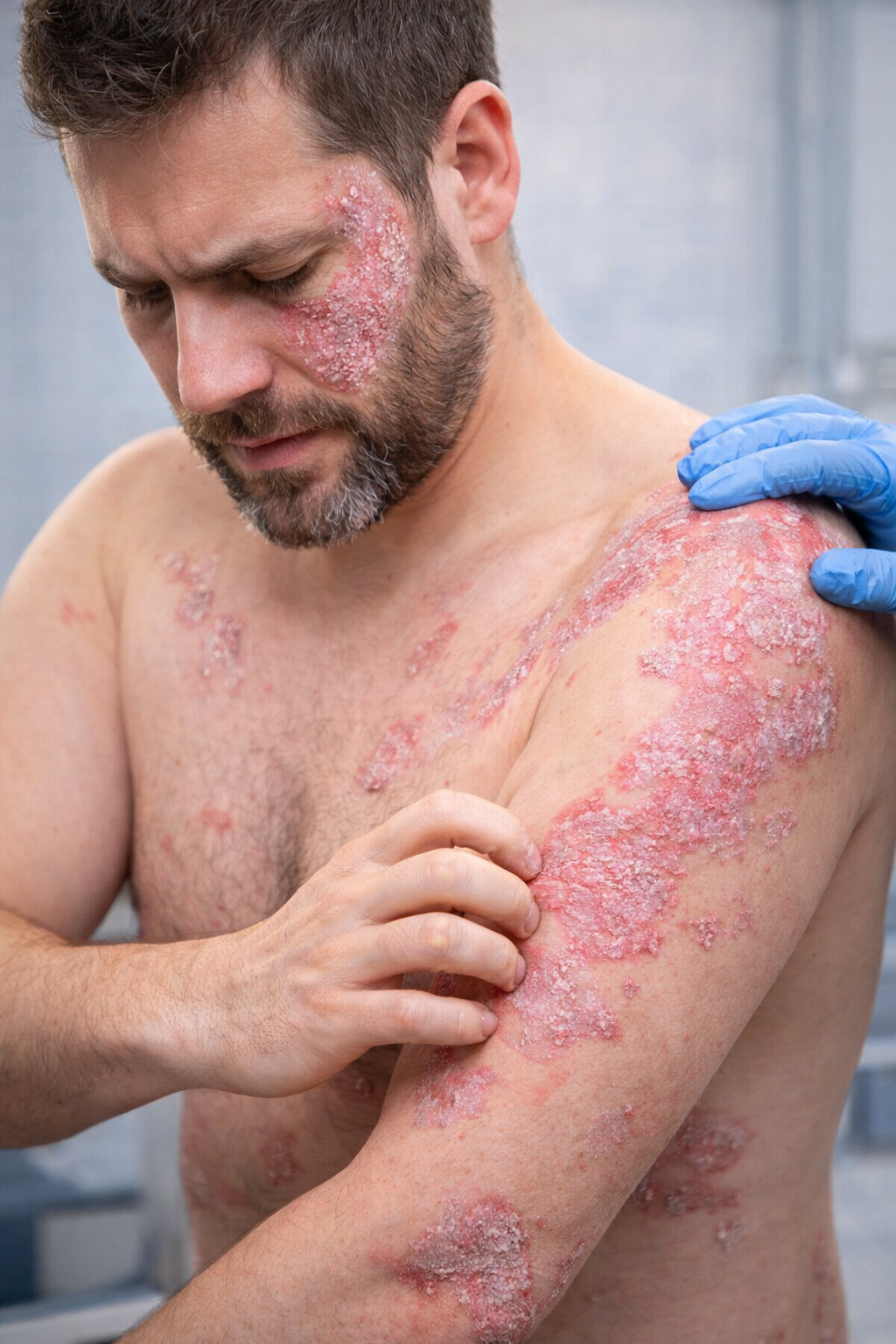
Flaking, itchy, scaly plaques on the face, trunk, and arms
Symptoms present for several months with worsening severity
Prior treatment with Humira (adalimumab) without sustained control
On exam:
Psoriasiform plaques with micaceous scale
Body Surface Area (BSA): 40% involvement
Itch severity: 8/10
Importantly, the patient denied joint pain, indicating no current signs of psoriatic arthritis.
What Is Psoriasis?
Psoriasis is a chronic autoimmune skin condition that speeds up skin cell turnover, leading to:
Thick, scaly plaques
Red or inflamed skin
Itching and discomfort
Common triggers include:
Stress
Infections (like strep throat)
Certain medications
Alcohol use
Psoriasis often follows a pattern of flares and remissions, requiring long-term management.
Why Do Some Treatments Stop Working?
Many patients ask why their psoriasis worsens even after biologic therapy.
The reality is:
The immune system can adapt or become less responsive to certain biologics over time
Missed or delayed doses can lead to disease flare-ups
Each biologic targets a different immune pathway, so switching may be necessary
In this case, the patient had been off Humira for over a year, contributing to a significant flare.
Advanced Treatment: Skyrizi (Risankizumab)
Given the severity and prior treatment failure, we initiated Skyrizi, a newer biologic therapy.
Why Skyrizi?
Targets IL-23, a key driver of psoriasis inflammation
Effective for moderate-to-severe psoriasis
Convenient dosing:
Week 0
Week 4
Then every 12 weeks
Supporting Treatments
While starting biologic therapy, we also recommended:
Topical Steroid
Triamcinolone ointment for flare control
Medicated Shampoo
Ketoconazole shampoo to manage scalp involvement
Skin Care Measures
Daily moisturizers
Controlled sun exposure
Anti-dandruff shampoos (zinc, selenium, tar)
Safety and Monitoring
Because biologics affect the immune system, proper screening is essential.
Baseline Labs Ordered:
Tuberculosis screening (QuantiFERON-TB Gold)
Hepatitis B & C testing
HIV screening
Complete blood count and metabolic panel
Ongoing Monitoring:
Annual TB testing
Watch for signs of infection
Patients are carefully counseled on risks such as immunosuppression and infection.
When Should You See a Dermatologist?
You should seek expert care if:
Psoriasis covers large areas of the body
Symptoms interfere with daily life
Treatments are no longer effective
You experience frequent or severe flares
Early intervention can significantly improve outcomes and quality of life.
Expert Psoriasis Care in Katy & Houston, TX
Village Dermatology provides advanced, personalized care for psoriasis patients across Katy and Houston, Texas, including:
Biologic therapy management
Comprehensive lab monitoring
Individualized treatment plans
Long-term disease control strategies
“Why Am I Getting Painful Red Skin Rashes and Bumps That Won’t Go Away?”
A 52-year-old patient in Katy, TX presented with persistent red rashes and painful cysts. Learn how intertrigo and epidermal cysts are diagnosed and treated by dermatologists.
By: Dr. Ashley Baldree
A Real Patient Case from Village Dermatology in Katy & Houston, Texas
Skin irritation in areas like the underarms, breast folds, or forearms can be frustrating—especially when symptoms persist for months. At Village Dermatology, we frequently evaluate patients with multiple skin concerns that may seem unrelated but are often connected.
This case highlights a 52-year-old female presenting with red skin lesions and a painful bump, ultimately diagnosed with intertrigo and an epidermal inclusion cyst.
Patient Case Overview
The patient came in with:
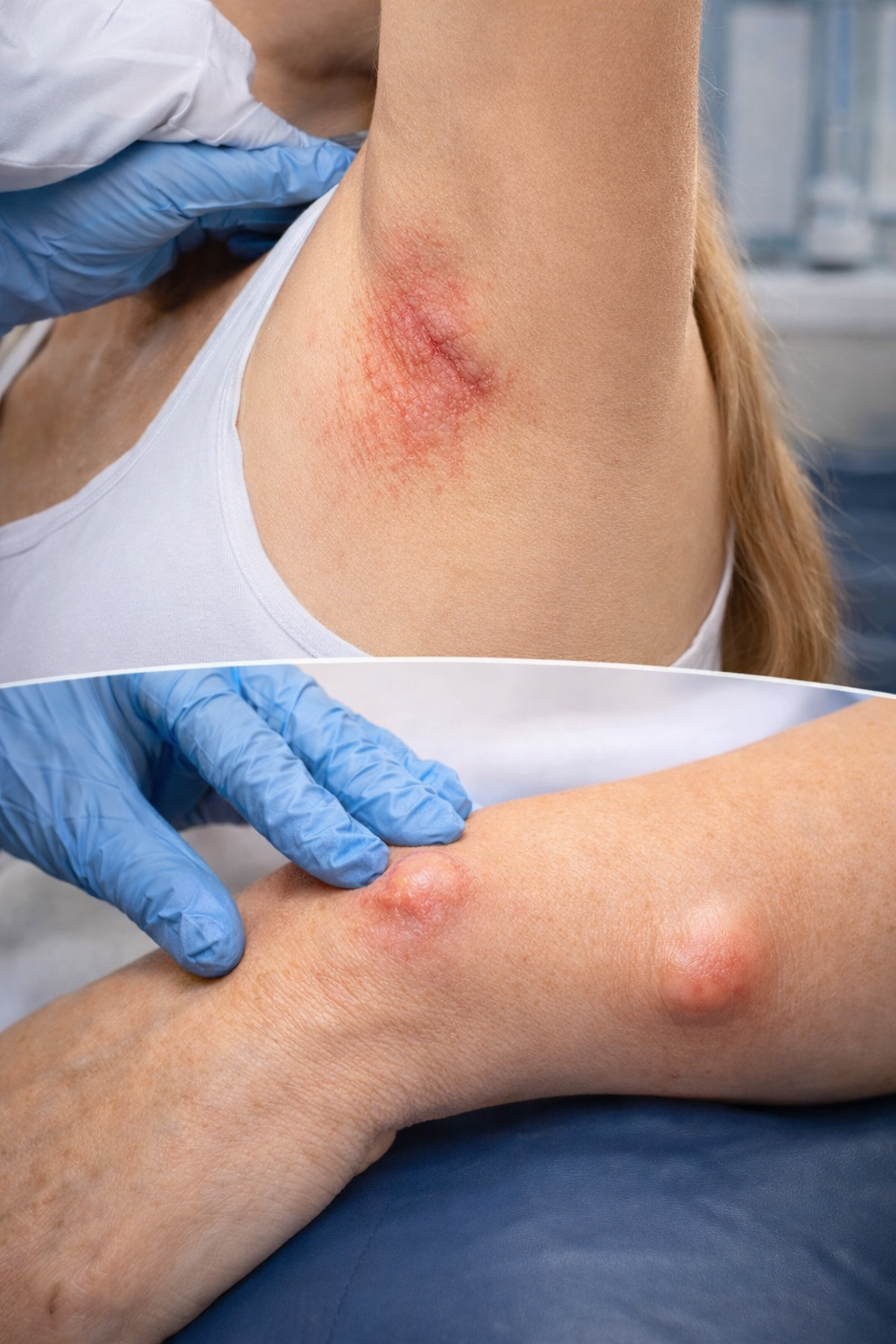
Red, inflamed skin lesions on the upper back, forearm, and underarm
A painful bump (cyst) on the forearm and breast
Symptoms present for several months without prior treatment
On examination:
The rash appeared consistent with intertrigo, a condition caused by friction and moisture
The bump was suspected to be an inflamed cyst vs. bug bite, later managed as a cyst
What Is Intertrigo?
Intertrigo is a common inflammatory skin condition that occurs in areas where skin rubs together, especially in warm, moist environments.
Common locations include:
Underarms
Under the breasts
Groin or abdominal folds
Symptoms:
Red, irritated patches
Burning or itching
Possible secondary fungal or bacterial infection
In this case, the patient’s underarm rash was consistent withintertrigo complicated by inflammation and possible fungal overgrowth.
What Is an Epidermal Inclusion Cyst?
An epidermal inclusion cyst is a benign, slow-growing lump beneath the skin filled with keratin.
Key features:
Round, firm bump under the skin
Can become painful, red, or infected
May require excision for complete removal
The patient’s cyst measured approximately 1 cm and caused discomfort, prompting treatment and planned removal.
Treatment Plan and Approach
At Village Dermatology, we take a comprehensive and targeted approach to treat multiple skin concerns simultaneously.
Intertrigo Treatment
Ketoconazole cream (antifungal) applied twice daily
Continued for 1 week after clearing to prevent recurrence
Recommended:
Barrier creams (zinc oxide/petrolatum)
Moisture control and friction reduction
Cyst Management (Forearm)
Vinegar soaks (1:1 vinegar + water) three times daily
Topical mupirocin antibiotic ointment applied after each soak
Cyst on Breast
Observation with plan for surgical excision if persistent
Why Do These Skin Conditions Occur Together?
Many patients are surprised to learn that:
Moisture, friction, and bacteria/fungus often work together to worsen skin conditions.
Intertrigo creates a compromised skin barrier
This environment allows microbial overgrowth
Cysts can become inflamed or infected in similar conditions
When Should You See a Dermatologist?
You should seek evaluation if:
Rashes persist for weeks or months
Skin becomes painful, swollen, or draining
A lump continues to grow or becomes tender
Early treatment can prevent complications and speed healing.
Expert Dermatology Care in Katy & Houston, TX
At Village Dermatology, we specialize in diagnosing and treating complex skin conditions, including rashes, infections, and cysts. Patients across Katy and Houston, Texas trust us for:
Accurate diagnosis with dermatoscopy
Personalized treatment plans
Medical and surgical dermatology expertise
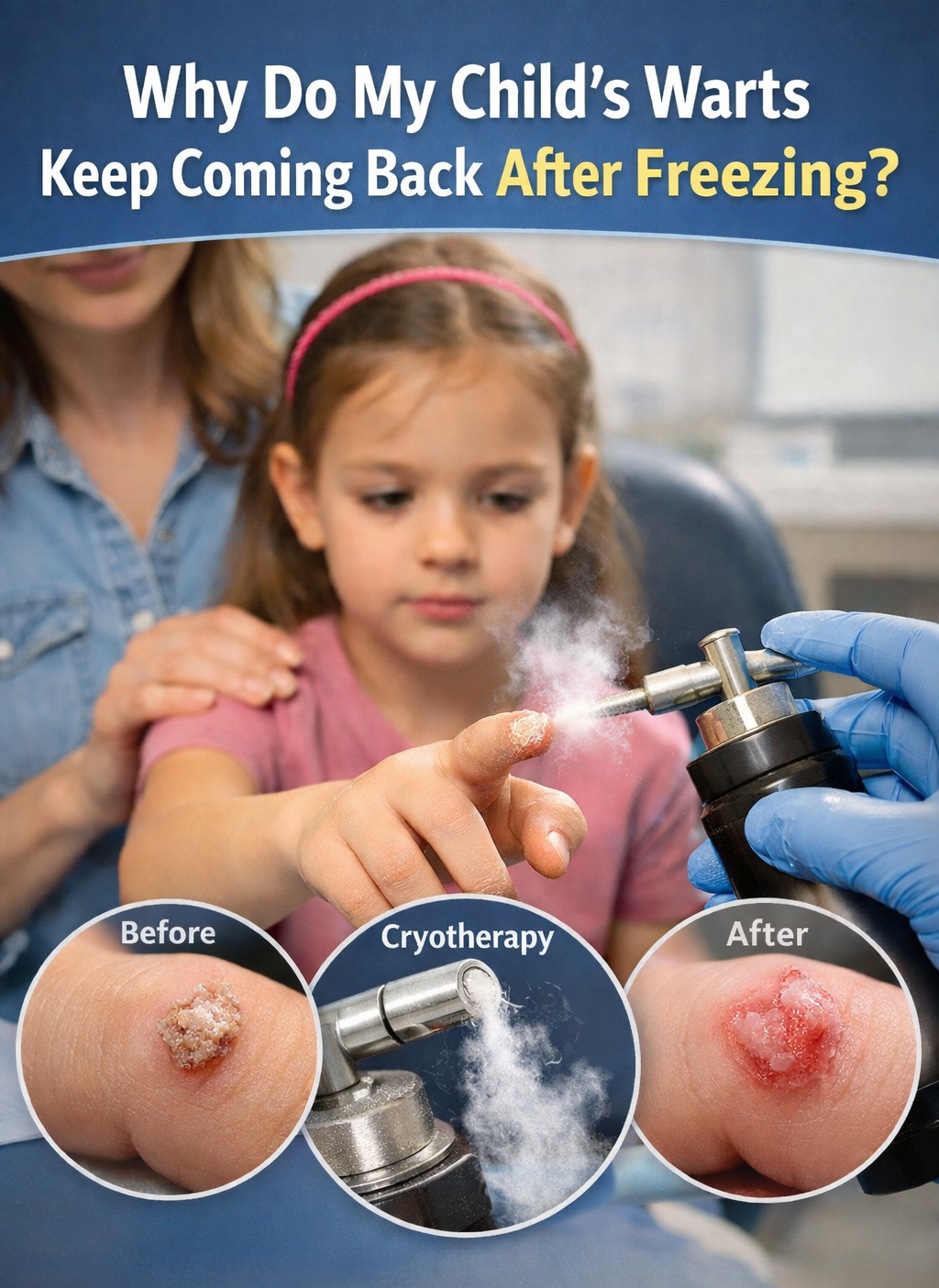
“Why Do My Child’s Warts Keep Coming Back Even After Freezing Them?”
A 7-year-old patient in Katy, TX presented with persistent warts despite cryotherapy. Learn why warts recur and how dermatologists in Houston effectively treat verruca vulgaris.
A Real Patient Case from Village Dermatology (Katy & Houston, Texas)
At Village Dermatology, we frequently see concerned parents asking why their child’s warts persist despite treatment. This recent case highlights a common—but treatable—skin condition known as verruca vulgaris (common warts).
Patient Case Overview
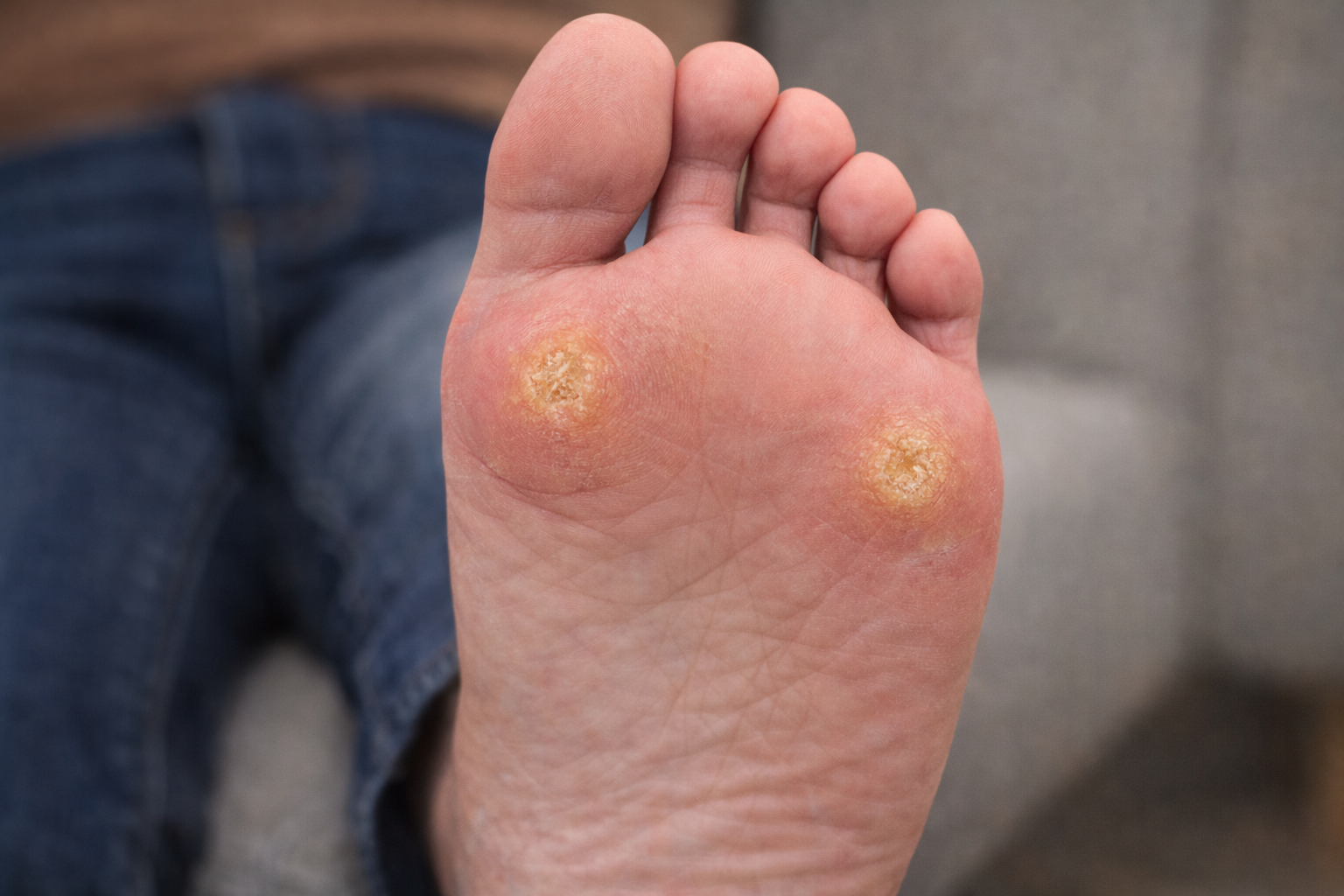
A 7-year-old female presented for follow-up evaluation of warts on her right hand, specifically on the ring finger and middle fingertip. She had previously undergone liquid nitrogen (cryotherapy) treatment about one month prior, with only mild improvement noted.
On examination, the lesions remained present and showed signs of:
Persistent growth
Mild inflammation
Thickened skin involvement near the nail
As part of treatment, careful trimming was performed to improve medication penetration, followed by another session of cryotherapy using liquid nitrogen.
What Are Verruca Vulgaris (Common Warts)?
Common warts are benign skin growths caused by the human papillomavirus (HPV). They often appear as:
Rough, cauliflower-like bumps
Skin-colored or slightly darker lesions
Found frequently on hands and fingers in children
They are contagious and can spread through:
Direct skin contact
Picking or scratching
Shared surfaces (e.g., towels, toys)
Why Didn’t the First Freezing Treatment Work Completely?
This is a very common concern. The truth is:
Warts often require multiple treatments.
Cryotherapy works by freezing the wart tissue, but:
Warts can extend deeper beneath the skin
The virus may persist even after visible improvement
Children’s immune systems respond at different speeds
In this case, the patient showed partial improvement, which is expected after just one session.
Treatment Approach at Village Dermatology
For this patient, we performed:
Cryotherapy (Liquid Nitrogen)
2 lesions treated
2 freeze–thaw cycles applied
Targeted destruction of wart tissue
Nail Trimming for Better Penetration
Helps treatment reach deeper viral tissue
Especially important for warts near or under nails
Education & Counseling
Families were advised that:
Multiple sessions are often needed
Warts may temporarily blister or scab after treatment
Recurrence is possible but manageable
Other Treatment Options for Warts
Depending on the case, we may also recommend:
Salicylic acid treatments (topical therapy)
Aldara (imiquimod cream)
Combination therapies for resistant warts
When Should You Follow Up?
You should return or contact your dermatologist if:
Warts are spreading quickly
They become painful or inflamed
There is no improvement after multiple treatments
In this case, the patient was scheduled for a 1-month follow-up to reassess response.
Why Choose Village Dermatology in Katy & Houston, TX?
At Village Dermatology, we specialize in treating pediatric and adult skin conditions with evidence-based, personalized care. Families across Katy and Houston, Texas trust us for:
Gentle pediatric dermatology care
Advanced wart removal techniques
Clear guidance for parents and patients
Compassionate, expert providers
“Why Do I Still Have Acne Scars Years Later—and Can They Actually Be Fixed?”
A 31-year-old patient visited Village Dermatology in Katy, Texas for long-standing acne scars. Learn how dermatologists treat acne scarring with CO2 laser, TCA CROSS, and PRP.
At Village Dermatology in Katy, Texas and Houston, Texas, one of the most common concerns we hear from patients is about acne scars that never seem to go away.
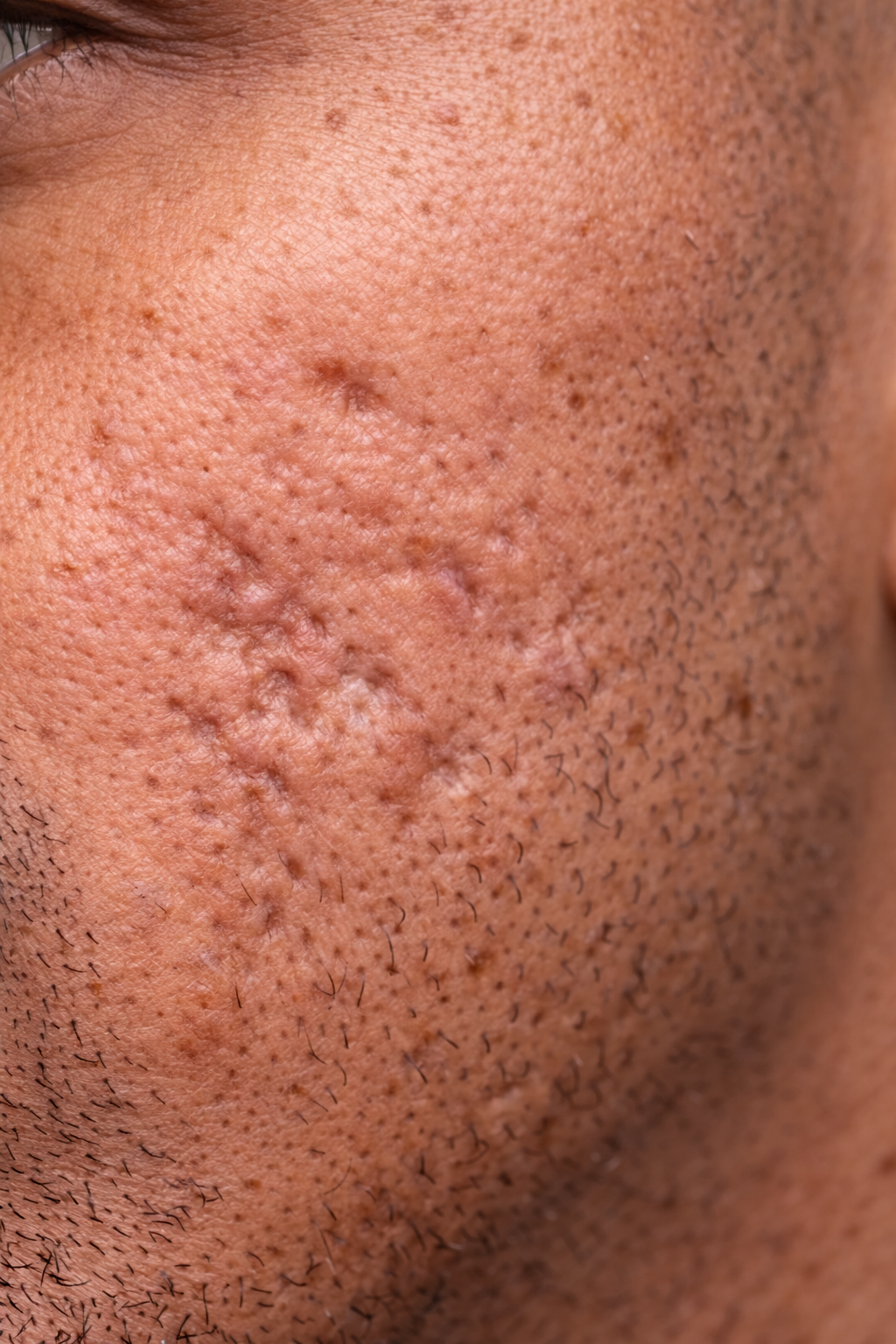
A 31-year-old male patient recently came to our clinic frustrated with long-standing acne scars on both cheeks. He had struggled with acne in the past and was left with noticeable scarring that had persisted for years.
During the visit, he asked a very relatable question:
“Why do I still have acne scars years later—and is there anything that can actually fix them?”
Understanding Acne Scarring
On examination, the patient had moderate to severe rolling acne scars on both cheeks.
These scars form when:
Deep inflammation damages the skin
Collagen is lost during healing
The skin surface becomes uneven or depressed
Rolling scars typically appear as:
Wave-like depressions in the skin
Uneven texture
Shadowing on the cheeks
Unlike active acne, scars are permanent structural changes in the skin, which is why they require specialized treatments.
Why Acne Scars Don’t Go Away on Their Own
Many patients expect scars to fade completely over time, but this is not always the case.
While some improvement can occur in the first 1–2 years, deeper scars often persist because:
The skin has lost underlying support (collagen)
The healing process was incomplete
Repeated inflammation worsened damage
This is why professional dermatologic treatments are often needed.
Previous Treatment: CO2 Laser
This patient had previously undergone two CO2 laser treatments, with the last session over a year ago.
He reported:
Significant improvement after treatment
But still had residual scarring
This is very common—most patients require multiple treatment modalities for optimal results.
Treatment Options for Acne Scars
We discussed several advanced treatment options to further improve his skin.
TCA CROSS
A targeted chemical reconstruction technique used for:
Deep acne scars
Ice-pick and rolling scars
It works by:
Stimulating collagen production
Gradually improving scar depth
PRP (Platelet-Rich Plasma)
PRP uses the patient’s own blood to:
Promote healing
Boost collagen production
Enhance results when combined with other treatments
CO2 Laser Resurfacing
A highly effective treatment that:
Resurfaces the skin
Stimulates new collagen
Improves overall texture
Often requires multiple sessions for best results.
Why Combination Treatment Works Best
For moderate to severe acne scarring, a combination approach is often recommended.
In this case, the patient was quoted a treatment plan including:
TCA CROSS
PRP
CO2 laser resurfacing
These treatments work together to:
Target different scar depths
Improve overall skin texture
Deliver more noticeable results
What About Topical Treatments?
We also discussed topical options such as tretinoin, which can help improve skin texture over time.
However, the patient reported sensitive skin and irritation with topicals, so we recommended:
OTC Adapalene (Differin Gel)
A milder retinoid
Helps with skin turnover
May improve texture gradually
Patients should discontinue use if irritation occurs.
Realistic Expectations for Acne Scar Treatment
It’s important for patients to understand:
Acne scars cannot be completely erased
Treatments aim to significantly improve appearance
Results take time and multiple sessions
Gradual improvement is expected over months
Consistency and patience are key.
When to See a Dermatologist
You should consider treatment if:
Acne scars affect your confidence
Skin texture is uneven
Over-the-counter products are not helping
You want more advanced cosmetic improvement
Acne Scar Treatment in Katy and Houston, Texas
At Village Dermatology, we offer advanced treatments for acne scarring including:
CO2 laser resurfacing
TCA CROSS
PRP therapy
Customized treatment plans
If you are struggling with persistent acne scars, our dermatology team can help you explore effective options for smoother, healthier skin.
“My Moles Haven’t Changed… So Why Do I Still Need to Get Them Checked?”
A 52-year-old patient followed up at Village Dermatology in Katy, Texas for stable moles. Learn why dermatologists still recommend routine skin checks even when moles haven’t changed.
By: Dr. Ashley Baldree
At Village Dermatology in Katy, Texas and Houston, Texas, one of the most common questions patients ask during follow-up visits is:
“If my moles look the same, do I really need to keep checking them?”
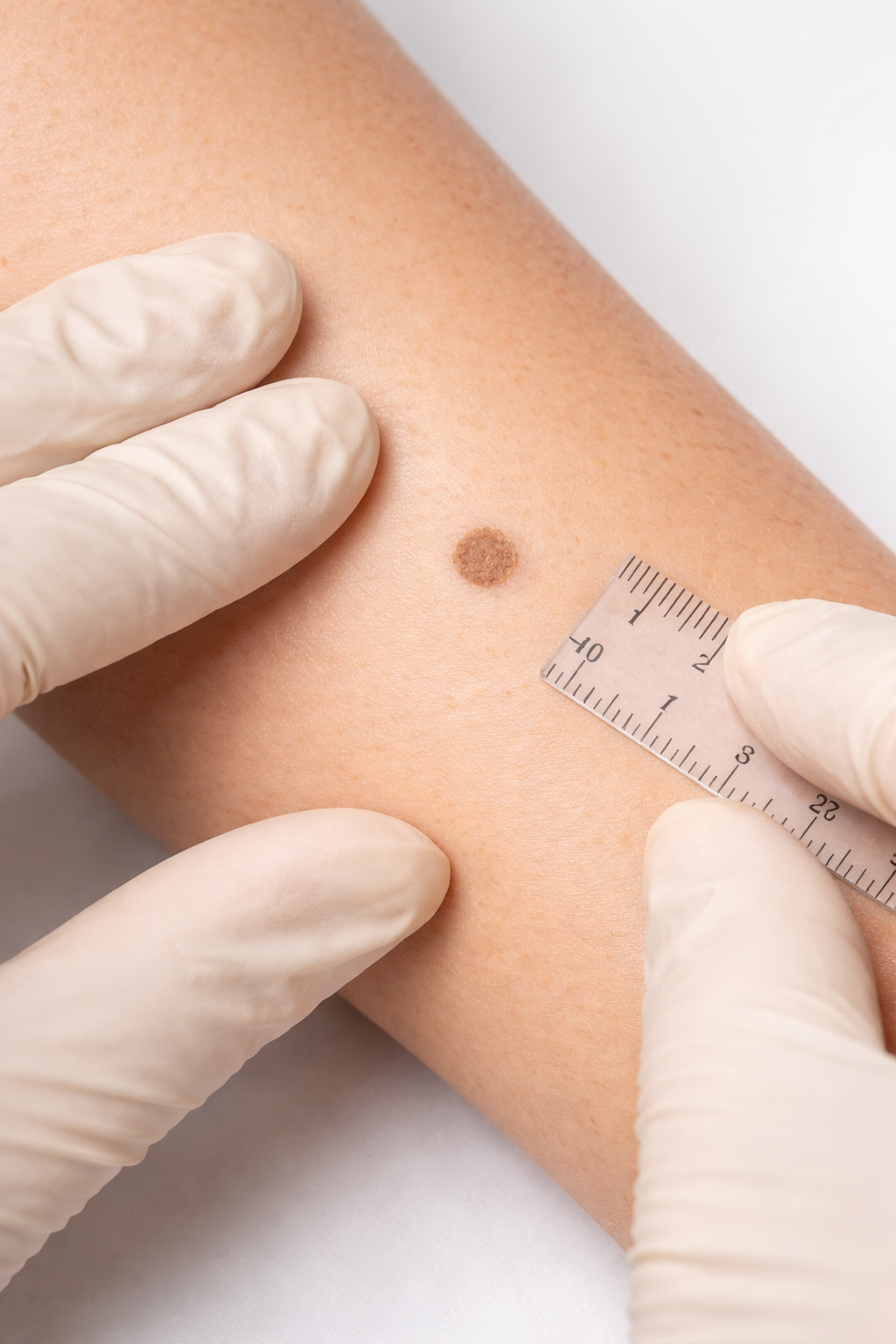
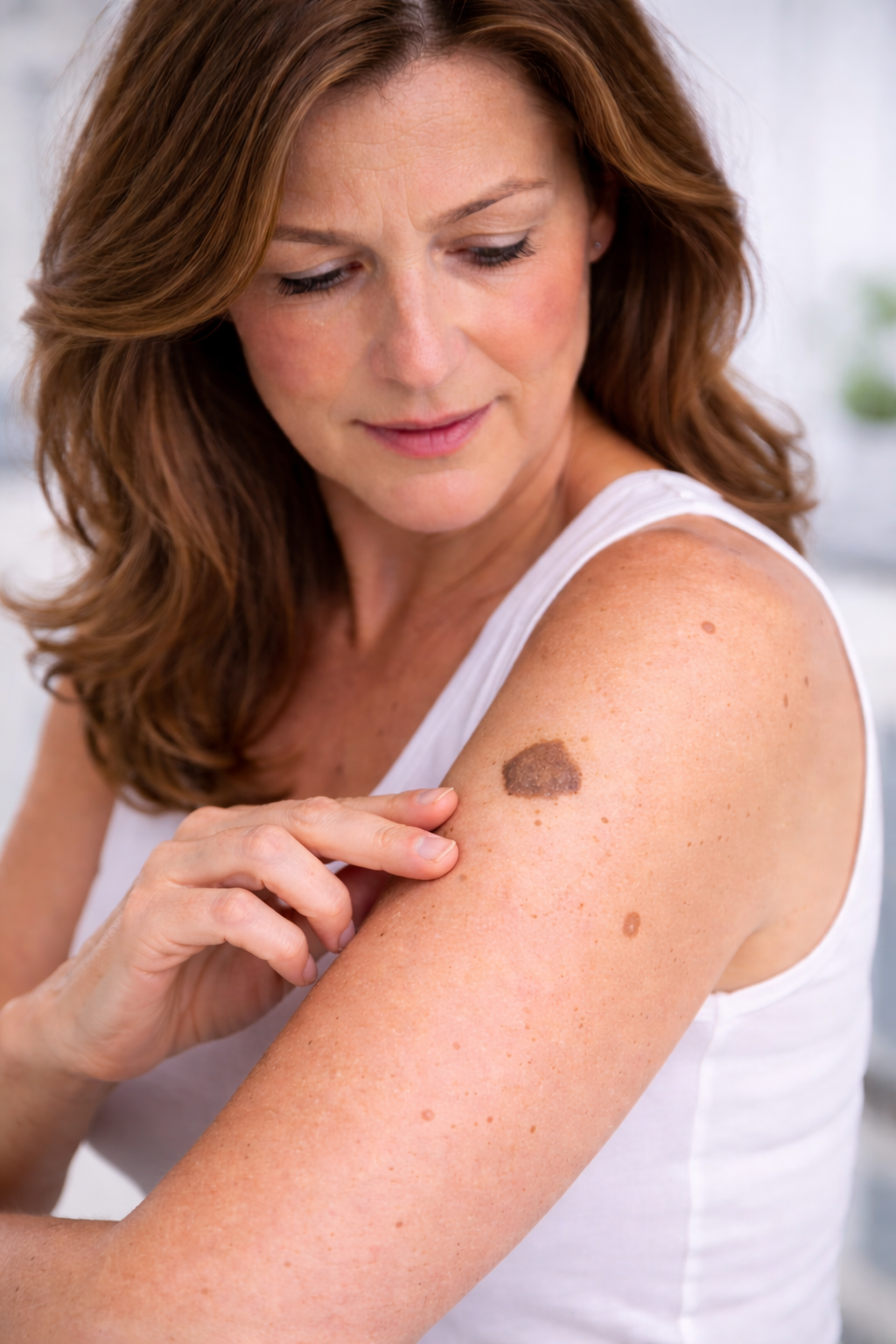
A 52-year-old female patient recently came in for a follow-up evaluation of benign moles (nevi) located on her body, including her left forearm and upper back. These moles had previously been measured and documented during her last visit.
Why Follow-Up Visits for Moles Matter
During this visit, a detailed skin examination was performed using a dermatoscope, allowing for close evaluation of the patient’s moles.
The previously monitored lesions measured:
4 mm on the left forearm
4.5 mm on the upper back
Importantly, both lesions remained:
Symmetrical
Evenly colored
Stable in size
These findings are consistent with benign nevi, meaning the moles are non-cancerous and do not require treatment.
However, even stable moles should continue to be monitored over time.
Why You Still Need to Monitor “Normal” Moles
Even when moles appear unchanged, dermatologists recommend continued surveillance because:
Skin changes can happen gradually and subtly
New moles or lesions may develop
Early skin cancer can mimic benign moles
A baseline comparison helps detect future changes
Regular monitoring ensures that any concerning changes are caught early, when treatment is most effective.
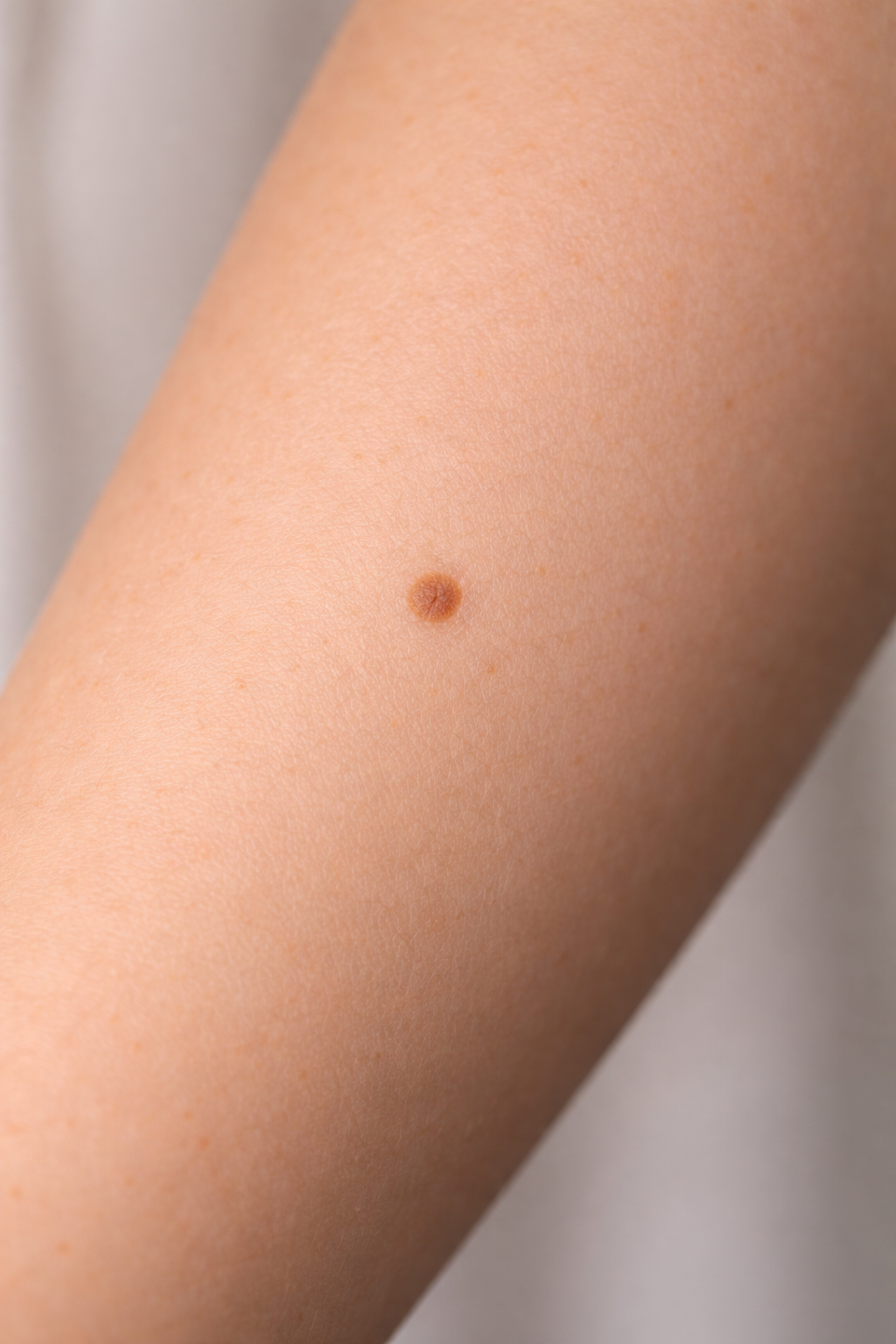
What Are Benign Nevi?
Benign nevi are extremely common and typically appear as:
Small brown or tan spots
Round or oval in shape
Evenly pigmented
Smooth borders
Most adults have multiple moles, and the majority remain harmless throughout life.
Other Common Skin Findings
During the exam, the patient also had additional benign skin conditions.
Lentigines (Sun Spots)
Lentigines are light brown spots caused by cumulative sun exposure.
They are commonly found on:
Arms
Face
Chest
Back
While harmless, they can be improved cosmetically with:
Retinoids
Chemical peels
Daily sun protection is key to preventing new spots.
Sebaceous Hyperplasia
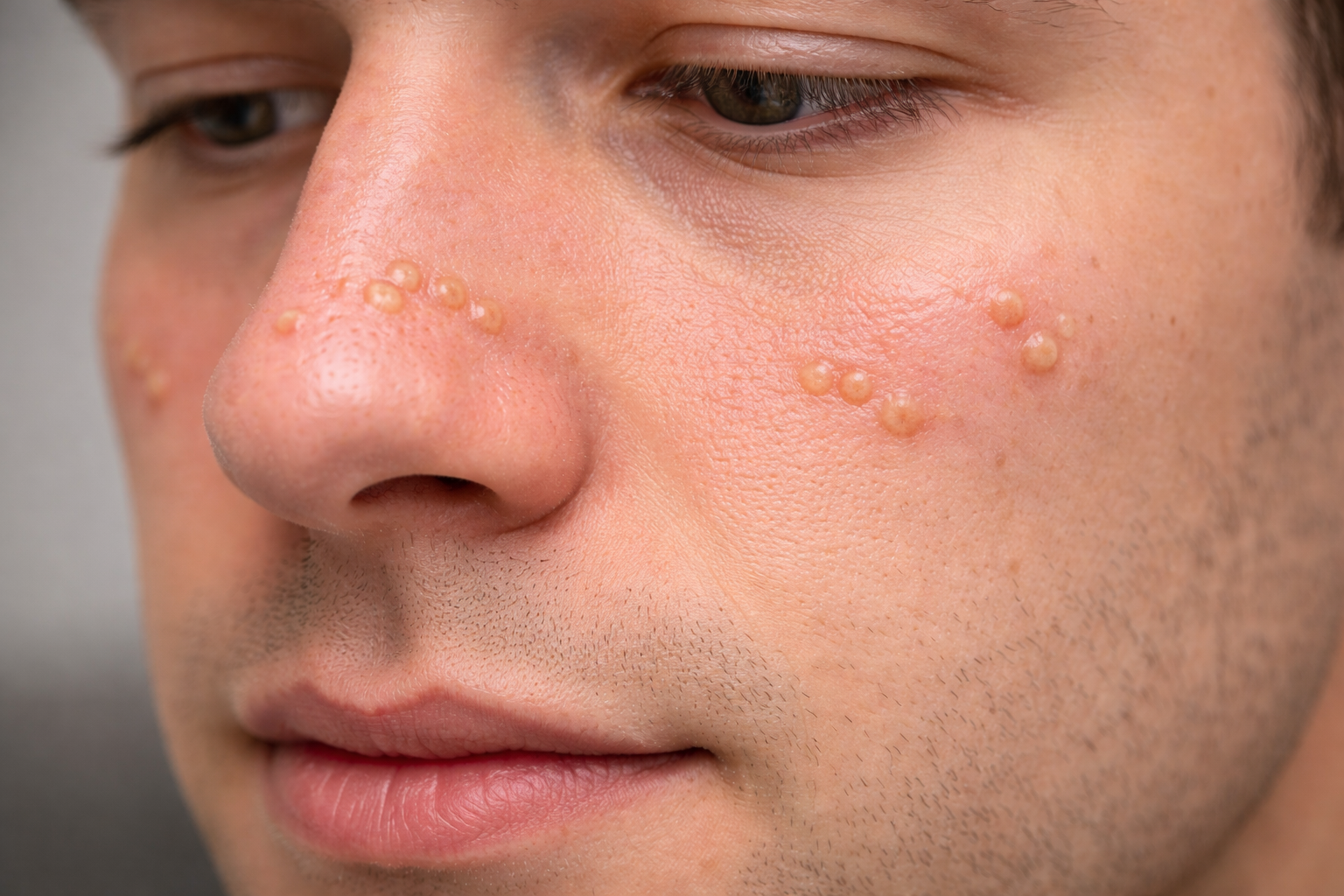
The patient also had sebaceous hyperplasia on the cheek.
These appear as:
Small yellow or flesh-colored bumps
Enlarged oil glands
Dome-shaped papules
They are completely benign and do not require treatment, but can be removed if desired using:
Laser therapy
Electrodessication
How to Check Your Moles at Home
Patients were advised to perform monthly self-skin exams.
Use the ABCDE rule when evaluating moles:
A – Asymmetry
B – Border irregularity
C – Color variation
D – Diameter (larger than 6 mm)
E – Evolving (changing over time)
If any mole changes in size, shape, color, or begins to itch or bleed, it should be evaluated promptly.
The Role of Sunscreen in Skin Health
Patients were strongly encouraged to use:
Sun-protective clothing when outdoors
Sunscreen helps:
Prevent new moles and sun spots
Reduce skin cancer risk
Protect against premature aging
When Should You See a Dermatologist?
You should schedule a skin exam if you notice:
New moles
Changes in existing moles
Spots that itch, bleed, or grow
Any lesion that looks different from others (“ugly duckling sign”)
Even without changes, annual skin checks are recommended.
Dermatology Care in Katy and Houston, Texas
At Village Dermatology, we specialize in:
Full-body skin exams
Mole monitoring and dermoscopy
Skin cancer screening and prevention
Treatment of benign skin lesions
If you have concerns about your moles or skin spots, our dermatology team is here to help.
“Do I Still Need Treatment If My Pre-Cancer Spots Look Better After PDT?”
A 63-year-old patient followed up at Village Dermatology in Katy, Texas after PDT treatment for actinic keratoses. Learn whether additional treatment is needed and how to prevent recurrence.
By: Dr. Ashley Baldree
At Village Dermatology in Katy, Texas and Houston, Texas, many patients return after treatment for precancerous skin lesions wondering what comes next. A 63-year-old male patient recently came in for a follow-up visit after undergoing photodynamic therapy (PDT) for actinic keratoses on the face.
At his appointment, he asked a very common and important question:
“Do I still need treatment if my pre-cancer spots look better after PDT?”
Follow-Up After Photodynamic Therapy (PDT)
This patient had previously been treated with red light photodynamic therapy, a highly effective treatment for actinic keratoses (AKs).
During his follow-up visit:
There was significant improvement
Previously visible lesions had markedly reduced
The patient reported no complications from treatment
Because of this excellent response, no additional treatment was needed at this time, and the plan was to continue routine monitoring.
What Are Actinic Keratoses?
Actinic keratoses are precancerous skin lesions that develop due to long-term sun exposure.
They typically appear as:
Rough, scaly patches
Red or pink spots
Areas that may feel like sandpaper
AKs are important to treat because a small percentage can progress to:
Squamous Cell Carcinoma (SCC)
Early treatment and follow-up significantly reduce this risk.
Do You Need Treatment After PDT?
Even when lesions improve or disappear, ongoing monitoring is essential.
Why?
New AKs can develop over time
Sun damage is cumulative
Some lesions may recur
If no active lesions are present, dermatologists often recommend:
Observation
Routine skin exams
Sun protection
Treatment is only restarted if new lesions appear.
How to Prevent Actinic Keratoses from Returning
Patients were counseled on the importance of sun protection:
Daily Prevention Tips
Use broad-spectrum sunscreen SPF 30+ every day
Wear sun-protective clothing and hats
Avoid peak sun hours when possible
Reapply sunscreen every 2 hours outdoors
Consistent sun protection is the most effective way to prevent recurrence.
Additional Diagnosis: Rosacea
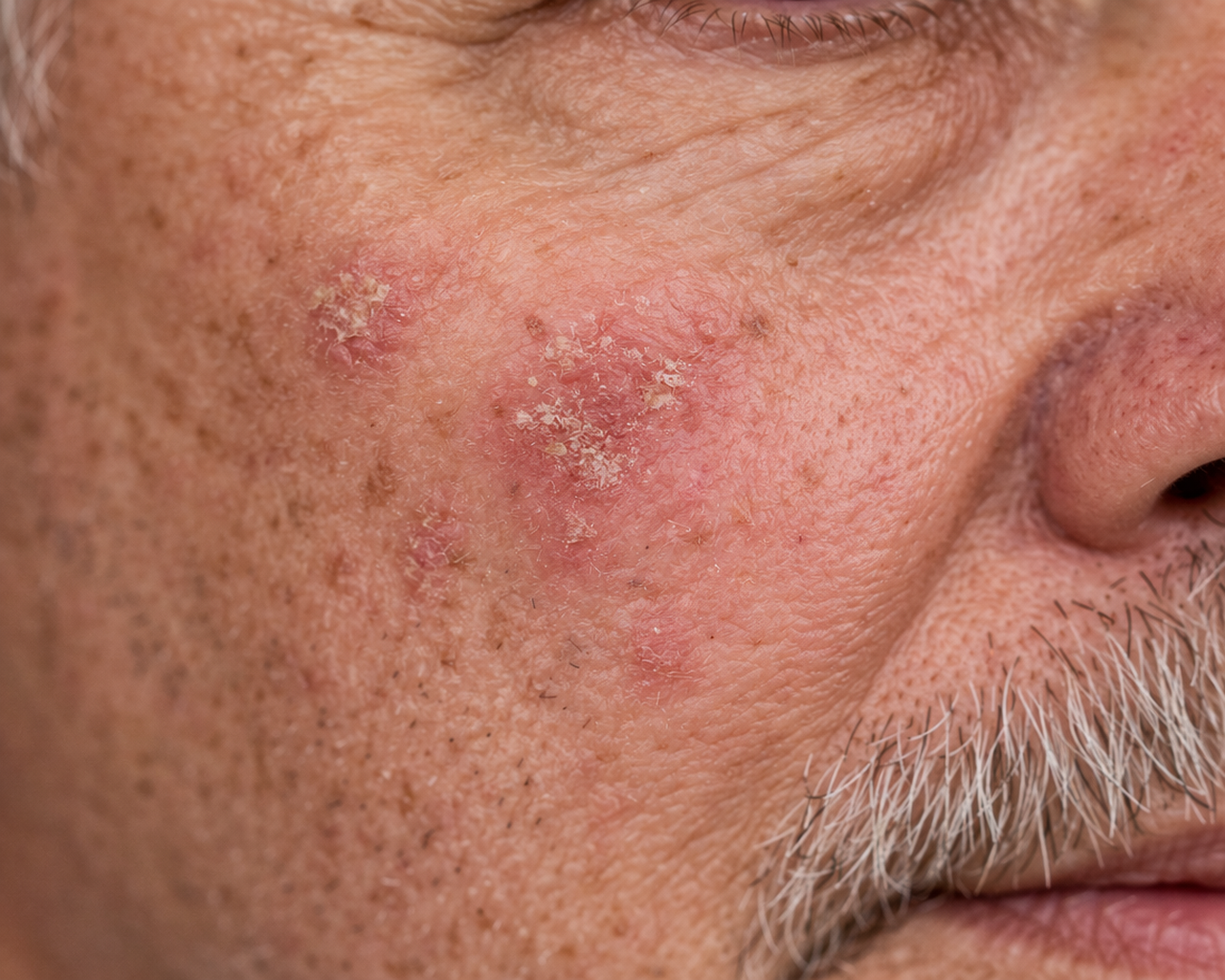
During the visit, the patient was also noted to have rosacea, a chronic inflammatory skin condition.
Symptoms included:
Redness
Acne-like bumps (papules and pustules)
Facial sensitivity
Treatment Plan for Rosacea
To help manage rosacea, the patient was started on:
Oral Doxycycline 20 mg
Taken twice daily with food
Helps reduce inflammation and breakouts
Topical Triple Cream
Applied nightly to the face
Helps control redness and lesions
Rosacea Triggers to Avoid
Patients were advised that rosacea can flare with:
Sun exposure
Heat
Spicy foods
Alcohol
Stress
Wind
Avoiding triggers can significantly reduce flare-ups.
When to Follow Up
The patient was scheduled to return in 3 months to reassess both:
Patients should return sooner if they notice:
New rough or scaly spots
Persistent redness or worsening bumps
Painful or non-healing lesions
Dermatology Care in Katy and Houston, Texas
At Village Dermatology, we specialize in:
Actinic keratosis treatment
Photodynamic therapy (PDT)
Rosacea management
Skin cancer prevention
Comprehensive skin exams
If you have sun-damaged skin, rough spots, or facial redness, our dermatology team can help you maintain healthy skin.
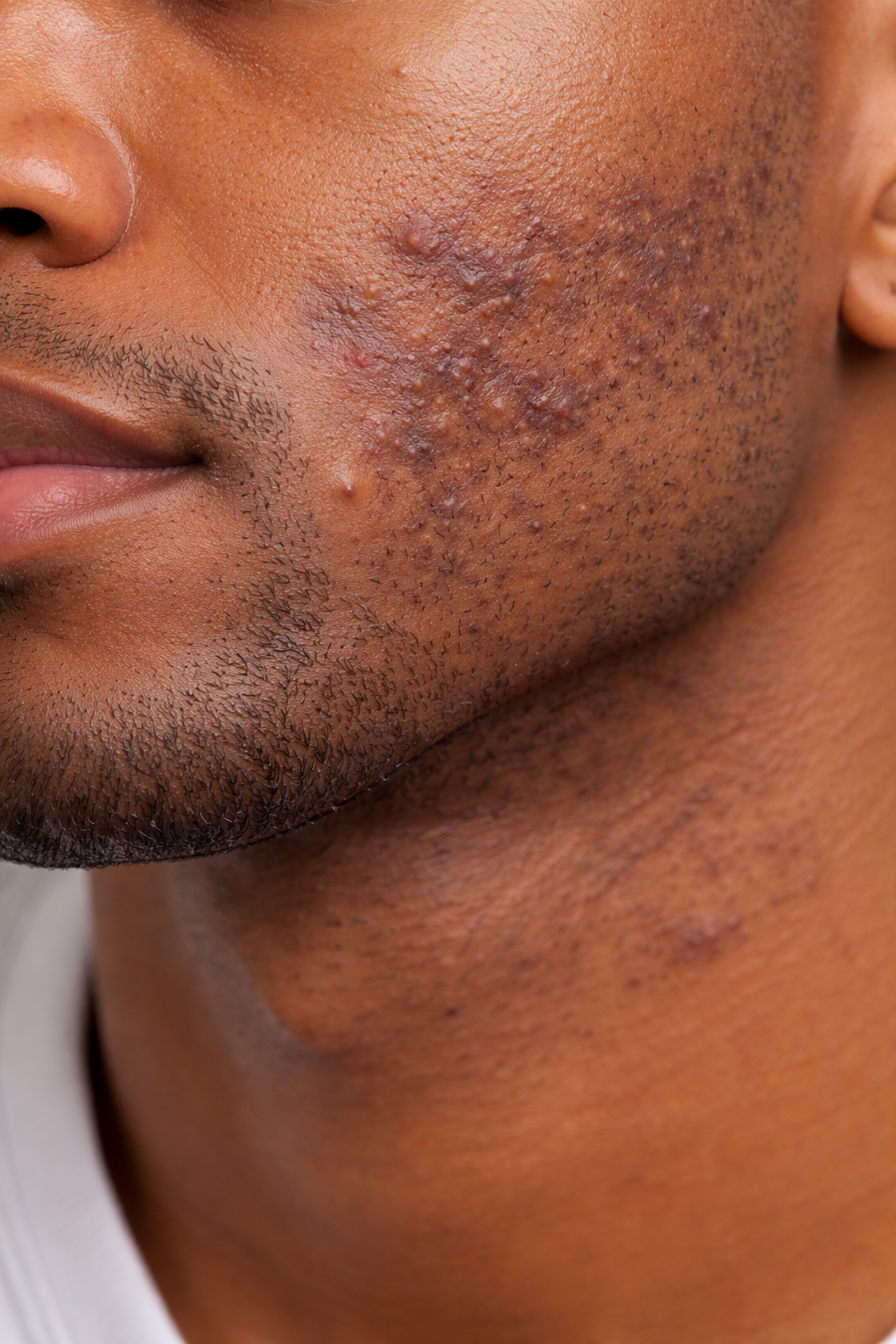
“How Do I Get Rid of Razor Bumps and Dark Spots on My Face?”
A 24-year-old patient visited Village Dermatology in Katy, Texas for dark spots and razor bumps. Learn how dermatologists treat pseudofolliculitis barbae and post-inflammatory hyperpigmentation.
At Village Dermatology in Katy, Texas and Houston, Texas, many young patients come in with concerns about dark spots and bumps on the face, especially after shaving.
A 24-year-old male patient recently visited our clinic with complaints of:
Brown discoloration on the cheeks
Recurrent bumps after shaving
Persistent skin changes that were not improving on their own
His main question during the visit was:
“How Do I Get Rid of Razor Bumps and Dark Spots on My Face?”
This is a very common concern, especially in patients with sensitive or curly facial hair.
Understanding Facial Hyperpigmentation
On examination, the patient had hyperpigmented patches on both cheeks, which are darker than the surrounding skin.
This condition is often referred to as post-inflammatory hyperpigmentation (PIH).
PIH occurs when the skin produces excess pigment after:
Irritation
Inflammation
Shaving-related trauma
These dark spots can take months to years to fade, especially without proper treatment and sun protection.
What Is Pseudofolliculitis Barbae (Razor Bumps)?
In addition to discoloration, the patient also had pseudofolliculitis barbae, commonly known as razor bumps.
This condition occurs when:
Hair curls back into the skin after shaving
The body reacts with inflammation
Small red or dark bumps form on the skin
It is most common in individuals with curly or coarse hair.
Symptoms may include:
Painful or itchy bumps
Dark spots after healing
Ongoing irritation with shaving
Why Razor Bumps Cause Dark Spots
Every time the skin becomes inflamed from ingrown hairs, it can leave behind post-inflammatory hyperpigmentation.
This creates a cycle:
Shaving causes irritation
Razor bumps develop
Skin heals with dark spots
New shaving leads to repeat irritation
Breaking this cycle is key to improving both bumps and discoloration.
Treatment Plan for Razor Bumps and Dark Spots
We developed a treatment plan to address both inflammation and pigmentation.
Morning Routine
Benzoyl Peroxide Wash (PanOxyl or CeraVe)
Helps reduce bacteria and inflammationClindamycin Gel
A topical antibiotic that treats inflamed bumpsSunscreen (SPF 30+)
Prevents dark spots from worsening
Evening Routine
Gentle Cleanser (La Roche-Posay)
Keeps skin clean without irritationTretinoin Cream
Helps by:Increasing skin turnover
Preventing clogged pores
Fading dark spots over time
Moisturizer (if needed)
Helps reduce dryness from treatment
Shaving Tips to Prevent Razor Bumps
Patients were counseled on proper shaving techniques to reduce irritation:
Shave with the grain, not against it
Avoid shaving too closely
Use clean, sharp razors
Consider electric clippers instead of razors
Avoid repeated passes over the same area
For long-term improvement, laser hair removal may be considered, as it can reduce hair growth and prevent ingrown hairs.
How Long Does It Take to See Improvement?
Patients should expect:
Improvement in bumps within a few weeks
Gradual fading of dark spots over several months
Continued improvement with consistent skincare and sun protection
If symptoms persist, additional treatments may be recommended.
Dermatology Care in Katy and Houston, Texas
At Village Dermatology, we specialize in treating:
Razor bumps (pseudofolliculitis barbae)
Hyperpigmentation
Acne and post-inflammatory skin changes
Chronic facial irritation
If you are experiencing persistent bumps or dark spots on your face, our dermatology team can create a personalized treatment plan to restore healthy skin.
“Should I Be Worried If My Moles Haven’t Changed Since My Last Skin Check?”
Concerned about moles or sun spots? Village Dermatology in Katy and Houston, Texas offers expert mole checks, skin cancer screenings, and dermatologic evaluations for suspicious skin lesions.
At Village Dermatology in Katy, Texas and Houston, Texas, many patients return for follow-up visits to monitor their moles and other skin spots. One of the most common questions dermatologists hear during these visits is:
“If my moles look the same as last year, do I still need to keep checking them?”
A 52-year-old female patient recently came in for a follow-up visit after previously being evaluated for benign moles (nevi) located on her body, including her left forearm and upper back.
She had been seen several months earlier, and photographs were taken to monitor the lesions. At this visit, the goal was to ensure the moles remained stable and showed no signs of skin cancer.
Monitoring Moles Over Time
During the follow-up visit, a dermatologic examination was performed using a dermatoscope, a specialized magnifying tool dermatologists use to examine skin lesions in detail.
The patient’s moles were carefully evaluated and documented.
Two specific lesions that were previously monitored included:
Left distal dorsal forearm – 4 mm mole
Left medial upper back – 4.5 mm mole
Both lesions remained:
Regular in shape
Symmetrical
Evenly pigmented
These characteristics are consistent with benign nevi, meaning the moles are non-cancerous and stable.
Because the lesions had not changed, the recommended approach was continued observation.
What Are Benign Nevi?
Benign nevi are very common skin growths composed of clusters of pigment-producing cells.
They typically appear as:
Small brown or tan spots
Evenly colored macules or papules
Symmetrical lesions with smooth borders
Most adults have 10 to 40 moles on their body, and they are usually harmless.
However, dermatologists recommend monitoring moles because changes over time can signal early skin cancer, particularly melanoma.
Why Dermatologists Take Photographs of Moles
At Village Dermatology, clinical photos may be taken to help monitor moles over time.
This allows dermatologists to:
Compare lesions during future visits
Detect subtle changes early
Avoid unnecessary biopsies when lesions remain stable
This approach is especially helpful for patients with multiple moles.
Other Common Skin Findings
In addition to benign moles, this patient had other common and harmless skin conditions.
Lentigines (Sun Spots)
Lentigines are light tan or brown spots caused by sun exposure.
They often appear on sun-exposed areas such as:
Face
Arms
Chest
Back
Although they are harmless, some patients choose treatment for cosmetic reasons.
Possible treatments include:
Retinoid creams
Chemical peels
Laser treatments
Skin-brightening products
Daily broad-spectrum sunscreen SPF 30 or higher is essential to prevent new spots from forming.
Sebaceous Hyperplasia
Another finding during the visit was sebaceous hyperplasia, located on the patient’s cheek.
Sebaceous hyperplasia occurs when oil glands enlarge and appear as:
Small yellow or flesh-colored bumps
Soft dome-shaped papules
Often located on the face
These lesions are completely benign and do not require treatment.
However, if desired, they can be treated with:
Electrodesiccation
Laser therapy
Topical retinoids
How to Monitor Your Moles at Home
Patients were advised to perform monthly self-skin exams to look for any changes in their moles.
Dermatologists recommend following the ABCDE rule when checking moles:
A – Asymmetry
B – Border irregularity
C – Color changes
D – Diameter larger than 6 mm
E – Evolving (changing over time)
If a mole begins to:
Grow
Change color
Become irregular
Itch, bleed, or become painful
it should be evaluated by a dermatologist.
The Importance of Annual Skin Exams
Even when moles appear normal, annual skin exams with a dermatologist are recommended.
Routine skin checks help detect:
Early melanoma
Basal cell carcinoma
Squamous cell carcinoma
Other suspicious lesions
Early detection greatly improves treatment outcomes.
Skin Monitoring and Dermatology Care in Katy and Houston, Texas
At Village Dermatology, we provide comprehensive skin evaluations including:
Full-body skin exams
Mole monitoring
Skin cancer screenings
Dermatoscopic evaluation
Treatment of benign and cosmetic skin lesions
If you have moles you want checked or changes in your skin, our dermatology team can help.
Schedule a skin exam at Village Dermatology in Katy or Houston, Texas to ensure your skin remains healthy.
“Why Do I Have Dark, Thick Patches on My Skin That Won’t Go Away?”
Struggling with thickened or discolored skin? Village Dermatology in Katy and Houston, Texas offers expert treatment for morphea, chronic rashes, and skin pigmentation disorders.
At Village Dermatology in Katy, Texas and Houston, Texas, patients often come to us with long-standing skin conditions that have not improved with prior treatments. One such case involved a 43-year-old female patient who presented with a chronic rash affecting multiple areas of her body.
Her main concern during the visit was:
“Why do I have dark, thick patches on my skin that won’t go away?”
This is a common question among patients dealing with morphea, a rare but persistent skin condition.
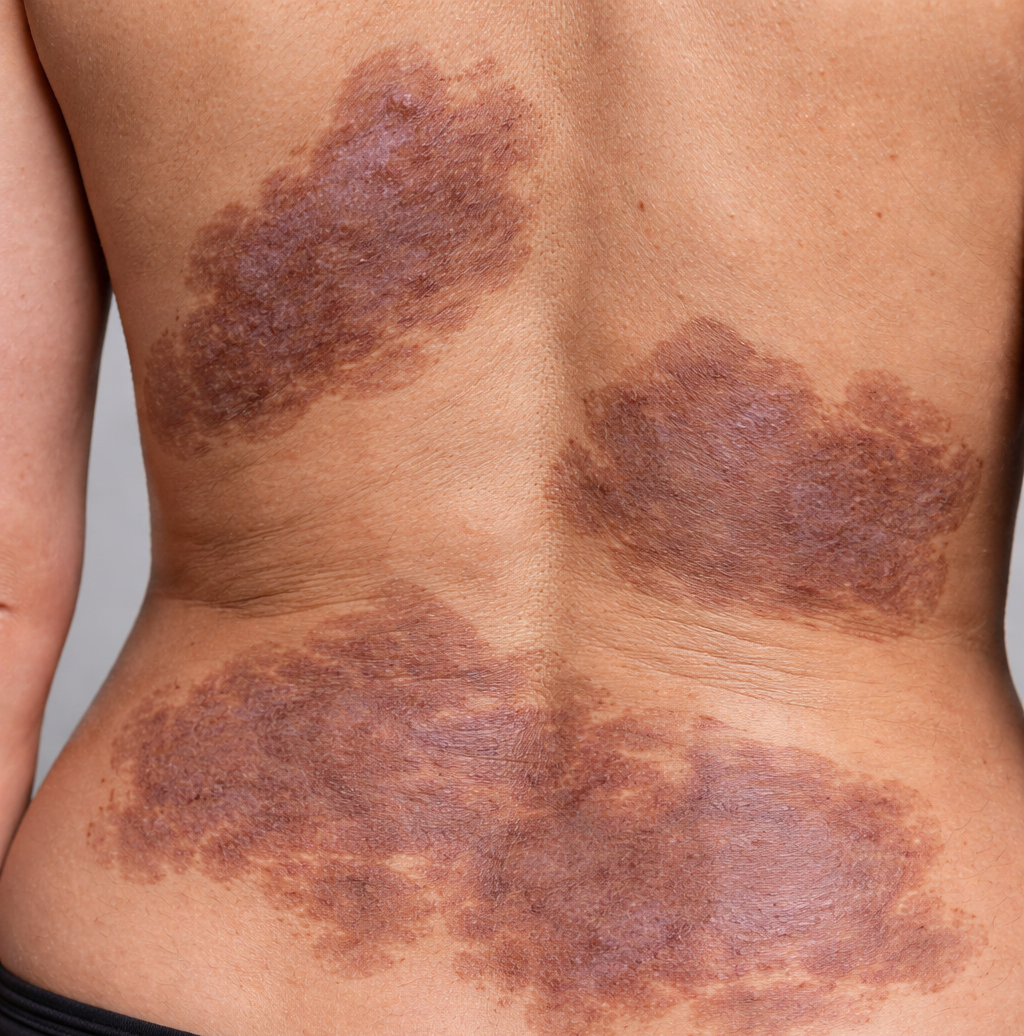
Understanding Generalized Morphea
During the examination, the patient was found to have generalized morphea, a condition she had previously been diagnosed with and treated for using phototherapy and systemic medications.
On exam, she had:
Confluent, bound-down hyperpigmented plaques
Areas of skin thickening (sclerosis)
Lesions distributed across the back, trunk, and breasts
Morphea is a type of localized scleroderma, which causes:
Hardening and thickening of the skin
Changes in pigmentation
Long-lasting plaques that may persist for years
Unlike systemic scleroderma, morphea typically does not affect internal organs, which is reassuring for many patients.
Why Morphea Can Be Difficult to Treat
Morphea can be challenging because:
It is chronic and long-lasting
Response to treatment can vary significantly
Lesions may improve slowly over time
Some areas may remain permanently changed
Even with treatment, patients may experience periods of progression and stability.
Treatment Options for Morphea
This patient had previously tried:
Methotrexate
Other light-based treatments
Given her ongoing symptoms, we discussed restarting treatment with a structured approach.
Phototherapy (Light Treatment)
Phototherapy is one of the most effective treatments for morphea.
The plan included:
Starting in-office phototherapy sessions
Initiating the process for at-home phototherapy approval
Phototherapy helps by:
Reducing inflammation
Softening thickened skin
Slowing progression of plaques
This treatment is often used long-term to manage symptoms.
Topical Treatments
Patients may also benefit from:
Topical steroids to reduce inflammation
Calcipotriene to help regulate skin cell growth
These treatments can improve the appearance and texture of affected skin.
Photoaging and Skin Health
In addition to morphea, the patient also had photoaging (sun damage) on the face.
Photoaging can cause:
Uneven pigmentation
Fine lines and wrinkles
Thinning of the skin
To address this, we recommended:
Tretinoin Benefits
Tretinoin helps by:
Increasing skin cell turnover
Improving skin texture
Reducing pigmentation and fine lines
Patients should:
Apply a pea-sized amount at night
Start 2–3 times per week
Increase gradually as tolerated
Cosmetic Treatment Considerations
The patient also expressed interest in cosmetic treatments. Given her diagnosis of morphea, we discussed safe options.
Safe Options:
Treatments to Avoid:
Laser resurfacing
These more aggressive treatments may worsen skin changes in patients with morphea.
When to Follow Up
Because morphea can evolve over time, the patient was advised to return in 2–3 months to monitor progress and adjust treatment as needed.
Patients should also contact their dermatologist if:
Lesions spread
Skin becomes more firm or thickened
New areas of involvement appear
Dermatology Care in Katy and Houston, Texas
At Village Dermatology, we specialize in treating complex and chronic skin conditions such as:
Morphea (localized scleroderma)
Chronic rashes
Pigmentation disorders
Photoaging and sun damage
If you are experiencing persistent skin changes that do not improve, our dermatology team can provide expert evaluation and personalized treatment.
Why Is This Rough Spot on My Nose Getting Bigger?
A 50-year-old woman visited Village Dermatology in Katy, Texas with a rough spot on the bridge of her nose that was enlarging. Learn how dermatologists diagnose and treat irritated seborrheic keratosis and other benign skin lesions.
By: Dr. Ashley Baldree
At Village Dermatology in Katy, Texas and Houston, Texas, patients frequently visit for evaluation of new or changing skin growths. A 50-year-old female recently came to our clinic concerned about a spot on the bridge of her nose that had slowly been enlarging over the past several months.
Her primary concern during the visit was:
“Why is this rough spot on my nose getting bigger?”
Because facial lesions can sometimes represent early skin cancers, careful dermatologic evaluation is essential.
This patient visit involved a full-body skin examination and dermoscopic evaluation of multiple lesions to rule out concerning growths. pasted
Full Skin Examination and Skin Cancer Screening
During the visit, a comprehensive skin exam was performed that included:
Scalp and hair
Face and eyelids
Ears and neck
Chest and abdomen
Back and extremities
Hands, feet, and nails
A dermatoscope was used to carefully examine the lesions and determine whether any required biopsy or treatment.
Fortunately, no signs of skin cancer were found. However, several common benign skin conditions were identified.
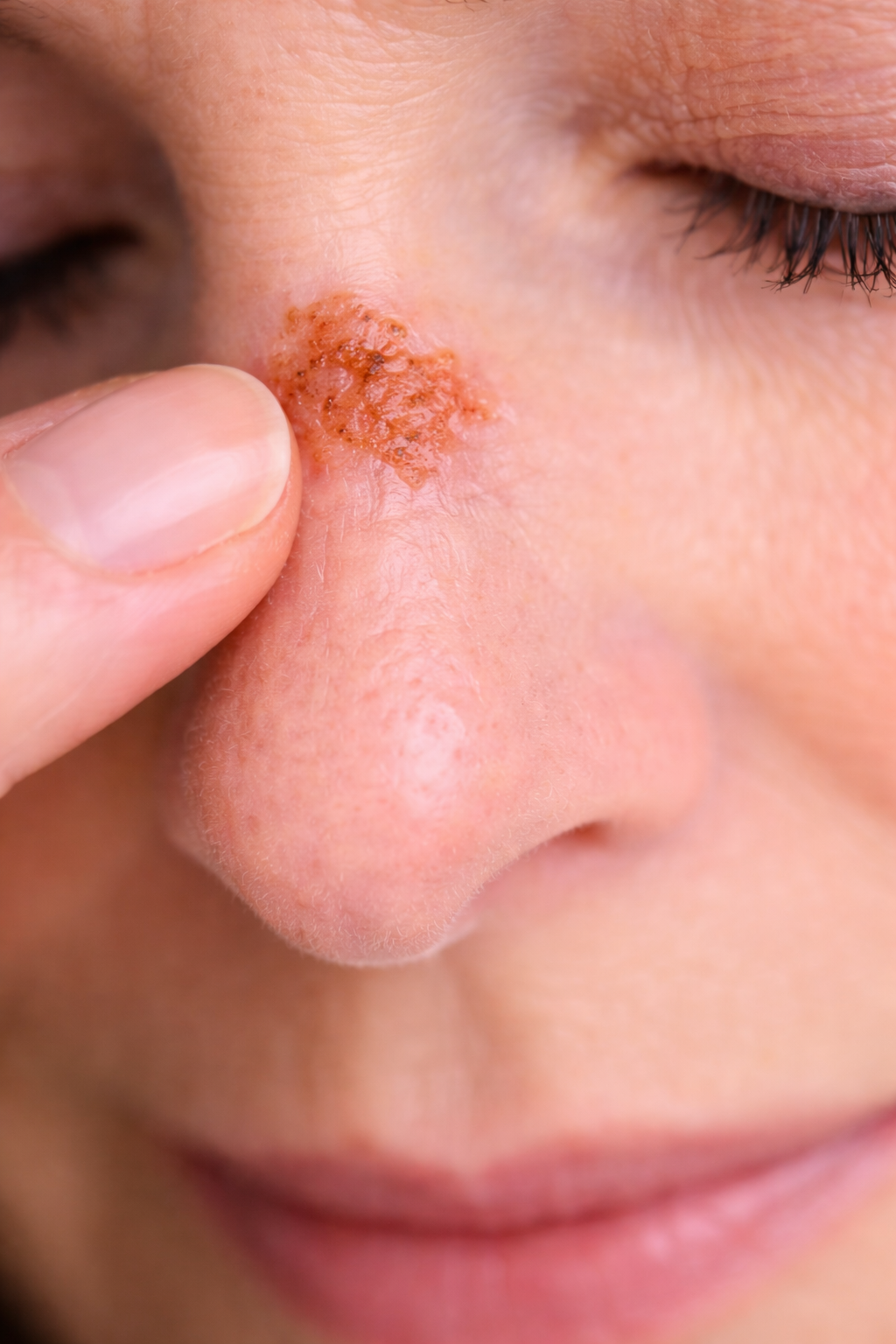
Irritated Seborrheic Keratosis on the Nose
The lesion that concerned the patient most was located on the nasal root (bridge of the nose).
It appeared as:
A stuck-on appearing papule
Slightly inflamed and crusted
Occasionally irritated
This lesion was diagnosed as an Irritated Seborrheic Keratosis (ISK).
Seborrheic keratoses are very common benign skin growths that often develop with age. They may appear:
Waxy
Slightly raised
Brown, tan, or skin colored
“Stuck-on” in appearance
When these lesions become inflamed or irritated, they can become red, itchy, or crusted.
Treatment: Liquid Nitrogen Cryotherapy
Because the lesion was irritated, the patient elected to treat it with cryotherapy using liquid nitrogen.
Cryotherapy works by:
Freezing the abnormal tissue
Causing the lesion to blister and fall off
Allowing healthy skin to regenerate
The lesion was treated with two freeze-thaw cycles of liquid nitrogen.
Patients are counseled that after cryotherapy they may experience:
Temporary redness
Crusting or blistering
Light or dark pigment changes
Mild scabbing as the skin heals
The patient was scheduled for follow-up in one month to ensure the lesion resolves appropriately.
Other Benign Skin Findings
During the skin exam, several additional benign lesions were noted.
Benign Nevi (Moles)
The patient had multiple benign nevi, which appeared as:
Regular
Symmetrical
Evenly pigmented
These are normal moles that do not require treatment, but patients should monitor them for any changes.
Lentigines (Sun Spots)
The patient also had lentigines, commonly known as sun spots.
These appear as:
Light tan macules
Areas of pigmentation on sun-exposed skin
They develop due to cumulative sun exposure over time.
Treatment options may include:
Retinoids
Chemical peels
Laser treatments
However, the most important preventative step is daily sunscreen use.
Cherry Angiomas
Small red vascular growths known as cherry angiomas were also observed.
These benign lesions:
Are extremely common
Increase with age
Require no treatment unless cosmetically bothersome
Prurigo Nodules
The patient also had prurigo nodules on the arms, which are thickened itchy nodules caused by repeated scratching.
Treatment focuses on breaking the itch-scratch cycle.
Recommended measures included:
Keeping nails trimmed short
Using moisturizers
Applying petroleum jelly (Vaseline)
Using anti-itch lotions if needed
Importance of Daily Sunscreen
Sun protection was strongly emphasized during this visit.
Patients were advised to use broad-spectrum sunscreen SPF 30 or higher.
Sunscreen tips include:
Apply 15 minutes before sun exposure
Reapply every 2 hours
Reapply sooner if sweating or swimming
Use approximately one ounce (shot glass amount) for full body coverage
Mineral sunscreens containing zinc oxide or titanium dioxide are excellent options for sensitive skin.
Recommended brands include:
EltaMD
ISDIN
Vanicream
CeraVe
Neutrogena Sheer Zinc
When Should You See a Dermatologist for a Skin Growth?
You should seek dermatologic evaluation if a lesion:
Is growing
Changes color or shape
Becomes irritated or crusted
Bleeds or does not heal
Even benign lesions can mimic skin cancer, which is why professional evaluation is important.
Expert Skin Lesion Evaluation in Katy and Houston, Texas
At Village Dermatology, our dermatology team provides expert care for:
Skin cancer screenings
Evaluation of suspicious skin growths
Seborrheic keratosis treatment
Mole monitoring and dermoscopy exams
Cryotherapy procedures
If you have a new or changing spot on your face or body, schedule a skin exam at Village Dermatology in Katy, Texas or Houston, Texas.
Early evaluation ensures peace of mind and protects your long-term skin health.
Should I Be Worried About All These Moles and Spots on My Skin?
A 50-year-old woman visited Village Dermatology in Katy, Texas for a full-body skin exam due to multiple moles and sun spots. Learn how dermatologists evaluate benign lesions and screen for skin cancer in Houston and Katy.
By : Dr. Caroline Vaughn
At Village Dermatology in Katy, Texas and Houston, Texas, many patients schedule routine skin exams because they notice new spots, moles, or skin changes. A 50-year-old female recently came to our office for a full-body skin check and evaluation of multiple skin lesions.
Her main concern during the visit was a question we hear often:
“Should I be worried about all these moles and spots on my skin?”
This is an important question because distinguishing between harmless skin growths and potential skin cancer requires expert evaluation.
Why Routine Skin Exams Are Important
The patient scheduled her visit for:
Evaluation of skin lesions throughout the body
Screening for suspicious growths
Education about sun exposure
Preventative skin cancer monitoring
She also reported a family history of non-melanoma skin cancer, which increases the importance of regular dermatology visits.
During the appointment, a comprehensive full-body skin exam was performed, including the scalp, face, neck, chest, back, arms, legs, hands, feet, and nails.
A dermatoscope was used to carefully evaluate moles and pigmented lesions.
Findings from the Skin Examination
Fortunately, the exam showed no signs of skin cancer. However, several common benign skin findings were identified.
These are extremely common in adults and increase with age and sun exposure.
Benign Nevi (Common Moles)
The patient had multiple benign nevi, which are normal moles.
These appeared as:
Regular, symmetrical spots
Evenly colored macules and papules
Stable pigmented lesions
Benign moles are clusters of pigment-producing cells within the skin and usually do not require treatment.
However, patients should monitor for any changes in:
Size
Shape
Color
Symptoms such as itching or bleeding
Monthly self-skin exams are recommended.
Lentigines (Sun Spots)
The patient also had lentigines, commonly called sun spots or age spots.
These appear as:
Light tan to brown macules
Reticulated pigmentation
Areas on sun-exposed skin
Lentigines develop from years of sun exposure and are very common in adults.
Although they are benign, they can be improved cosmetically with:
Sunscreen use
Retinoids
Chemical peels
Laser treatments
Preventing further sun damage is key.
Seborrheic Keratoses
Another finding was seborrheic keratoses, which are very common benign growths.
They typically look like:
Waxy or "stuck-on" growths
Brown, black, or tan lesions
Slightly raised textured plaques
These growths are harmless and do not require treatment, though they can be removed for cosmetic reasons.
During this visit, the patient elected to defer treatment of one lesion on the cheek.
Cherry Angiomas
The exam also revealed cherry angiomas, which are small benign blood vessel growths.
They appear as:
Bright red spots
Dome-shaped papules
Smooth vascular lesions
Cherry angiomas are extremely common and increase with age.
Treatment is not necessary, but they can be removed with:
Laser therapy
Electrodessication
Skin Cancer Risk and Family History
Because the patient has a family history of non-melanoma skin cancer, we discussed several important preventative steps.
These include:
Using sun protective clothing
Avoiding excessive sun exposure
Performing monthly self-skin examinations
Family history can increase the risk of developing skin cancer, which makes regular dermatology screenings essential.
How to Perform a Self-Skin Exam
Patients should examine their skin monthly and watch for:
New spots that appear suddenly
Moles that change shape or color
Lesions that bleed or do not heal
Rapidly growing bumps
Any suspicious changes should be evaluated by a dermatologist promptly.
How Often Should You Have a Full Body Skin Exam?
For most adults, dermatologists recommend annual full-body skin exams.
However, people with risk factors such as:
Family history of skin cancer
Numerous moles
Significant sun exposure
Fair skin
may benefit from more frequent screenings.
Expert Skin Cancer Screening in Katy and Houston, Texas
At Village Dermatology, our dermatology team specializes in:
Skin cancer screenings
Mole evaluation
Dermoscopy examinations
Preventative dermatology
Treatment of benign skin growths
If you have moles, spots, or new skin lesions, a professional skin exam can provide peace of mind.
Schedule your annual skin check at Village Dermatology in Katy or Houston, Texas today.
Early detection saves lives.
Why Are My Feet Always Peeling and Itchy?
A 77-year-old male presented to Village Dermatology in Katy, Texas with chronic itchy, peeling feet caused by tinea pedis (athlete’s foot). Learn how dermatologists in Houston and Katy diagnose and treat fungal foot infections.
By: Dr. Caroline Vaughn
At Village Dermatology in Katy, Texas and Houston, Texas, we frequently see patients who struggle with chronic foot rashes that never seem to completely go away. A 77-year-old male recently came to our office with a long history of itchy, red, peeling skin on his feet that had been occurring intermittently for years.
During the visit, he asked an important question many patients have:
“Why are my feet always peeling and itchy even after using steroid cream?”
After a detailed exam, we were able to identify the underlying issue and develop a more effective treatment plan.
Patient Case: Chronic Rash on the Feet
This patient presented with:
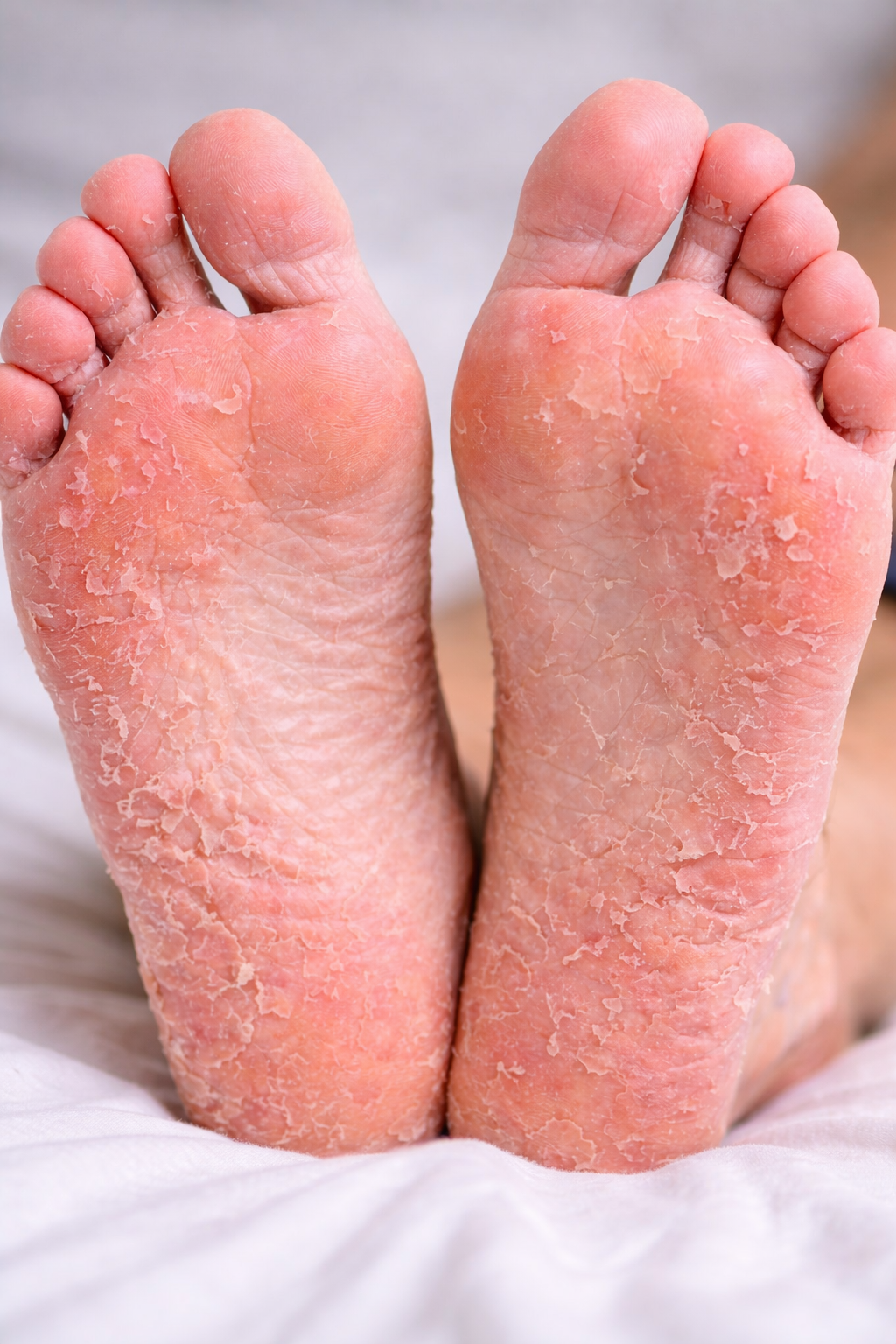
Peeling and scaling skin on the feet
Redness and itching
Symptoms present intermittently for several years
No recent infections or new products
No household contacts with similar symptoms
During the physical exam, we observed scaling and peeling on the plantar forefoot of both feet, along with severe toenail fungus (onychomycosis).
The findings were most consistent with:
Tinea Pedis (Athlete’s Foot)
What Is Tinea Pedis?
Tinea pedis is a fungal infection of the skin on the feet, commonly known as athlete’s foot.
It occurs when dermatophyte fungi grow in warm, moist environments such as:
Shoes
Locker rooms
Pools
Humid climates
Common symptoms include:
Peeling skin
Scaling
Itching
Redness
Cracked skin
Although treatment is often effective, recurrence is common, especially in older adults.
Why Steroid Cream Made the Problem Worse
The patient had been using triamcinolone 0.1% cream, a topical steroid.
While steroids can help inflammation, they do not treat fungal infections.
In fact, topical steroids may:
Suppress the immune response
Allow fungus to spread more easily
Mask symptoms temporarily
This is a common reason chronic fungal infections go untreated for years.
Treatment Plan for Athlete’s Foot
At Village Dermatology in Katy and Houston, Texas, we recommended a step-by-step treatment approach.
Step 1: Treat the Fungal Infection
The patient was advised to start:
Over-the-counter terbinafine (Lamisil) cream
Apply twice daily for 2 weeks
Targets the fungal infection directly
Helps eliminate athlete’s foot
Important note: this treatment will not treat toenail fungus, which often requires different therapy.
Step 2: Address Scaling and Thickened Skin
After antifungal therapy is completed:
Resume triamcinolone 0.1% ointment if inflammation persists
Begin urea 40% cream to soften thickened skin and reduce scaling
Urea works by gently breaking down thick keratin buildup.
Severe Toenail Fungus: Why a Podiatry Referral Was Recommended
The patient also had severe onychomycosis (toenail fungus).
Toenail fungus is difficult to treat because:
The fungus lives beneath the nail plate
Topical medications often cannot penetrate deeply enough
For long-term management, we recommended referral to a podiatrist.
Treatment options may include:
Oral antifungal medications
Nail debridement
Laser treatment in some cases
Hyperkeratosis of the Feet
In addition to the fungal infection, the patient also had hyperkeratosis, a condition where the skin becomes thick and scaly.
Hyperkeratosis can develop from:
Chronic friction
Dry skin
Recurrent inflammation
Aging skin changes
Treatment focuses on:
Regular moisturization
Keratolytic creams such as urea
Gentle exfoliation
How to Prevent Athlete’s Foot from Returning
Because recurrence is common, we recommend several preventative steps:
Keep feet dry
Change socks daily
Wear breathable footwear
Use antifungal powders if prone to recurrence
Avoid walking barefoot in public locker rooms or pools
These small habits can significantly reduce reinfection.
When Should You See a Dermatologist for Foot Rash?
You should seek evaluation if:
Foot rash lasts longer than a few weeks
Steroid creams are not helping
Toenails become thick or yellow
The rash keeps coming back
Skin cracks or becomes painful
A dermatologist can determine whether the cause is fungal infection, eczema, psoriasis, or another skin condition.
Expert Athlete’s Foot Treatment in Katy and Houston, Texas
At Village Dermatology, our dermatology team provides expert care for:
Toenail fungus
Chronic foot rashes
Hyperkeratosis
Inflammatory skin conditions
If you are experiencing itchy, peeling feet or persistent foot rash, schedule an appointment with Village Dermatology in Katy, Texas or Houston, Texas.
Early diagnosis and proper treatment can restore healthy skin and prevent chronic recurrence.
Why Are Dark Patches Showing Up on My Cheeks After an Eyelid Rash?
A 40-year-old woman presented to Village Dermatology in Katy, Texas with dark cheek discoloration following an eyelid rash. Learn about post-inflammatory hyperpigmentation treatment and expert dermatologic care in Houston and Katy, TX.
At Village Dermatology in Katy, Texas and Houston, Texas, we often see patients who are concerned about sudden changes in their skin tone. A 40-year-old woman recently came to our office worried about darker patches developing on both cheeks over the past several weeks.
Her main question during the visit was:
“Why are dark patches showing up on my cheeks after my eyelid rash?”
Let’s break down what was happening and how we treated it.
Case Overview: Skin Discoloration on the Cheeks
This patient presented with:
Darker-than-normal skin patches on the right and left cheeks
Moderate discoloration
Symptoms present for several weeks
A recent history of rash around the eyelids
On examination with dermoscopy, we noted ill-defined hyperpigmented patches consistent with:
Post-Inflammatory Hyperpigmentation (PIH)
The discoloration was secondary to inflammation from her recent eyelid dermatitis.
What Is Post-Inflammatory Hyperpigmentation (PIH)?
Post-inflammatory hyperpigmentation occurs when the skin produces excess pigment after inflammation or irritation.
Common triggers include:
When inflammation resolves, it may leave behind:
Dark brown patches
Gray-brown discoloration
Uneven skin tone
PIH is especially common in individuals with medium to darker skin tones but can affect all skin types.
Why Did the Eyelid Rash Cause Cheek Discoloration?
This patient also reported:
Rash under the eyes
Onset during seasonal allergy flare
No new skincare products
She was diagnosed with:
Eyelid Dermatitis
Eyelid skin is extremely thin and sensitive. Allergies, rubbing, and inflammation can trigger dermatitis, which may spread or cause pigment changes in nearby areas like the cheeks.
Even after the rash improves, pigmentation can linger for months.
Treatment Plan at Village Dermatology
At Village Dermatology in Katy and Houston, Texas, we treat both the inflammation and the pigmentation to restore healthy, even skin tone.
1. Treat the Eyelid Dermatitis
We prescribed:
Elidel (pimecrolimus) 1% cream
Apply once daily to eyelids
Elidel is a non-steroidal anti-inflammatory cream that is safe for delicate eyelid skin.
We also recommended:
Daily Zyrtec for allergy control
Discontinuing all skincare products temporarily
Using only hypoallergenic, fragrance-free products
If no improvement, we discussed the possibility of switching to Opzelura.
2. Treat the Post-Inflammatory Hyperpigmentation
For pigmentation management, we recommended:
Broad Spectrum Sunscreen SPF 30+ (daily use)
Sun protective clothing
Topical retinoids to encourage skin cell turnover
Sun exposure can worsen hyperpigmentation and delay fading. Consistent sunscreen use is critical.
How Long Does Post-Inflammatory Hyperpigmentation Last?
We counseled the patient that:
PIH can take months to years to fully fade
Improvement is gradual
Early treatment improves outcomes
Strict sun protection is essential
Patience and consistent treatment are key.
When Should You See a Dermatologist for Facial Discoloration?
You should seek evaluation if:
Dark patches appear suddenly
Pigmentation follows a rash
Discoloration is spreading
Over-the-counter creams are not working
The rash keeps recurring
Proper diagnosis is important because facial pigmentation can also represent:
Melasma
Lichen planus pigmentosus
Drug reactions
Chronic dermatitis
Expert Pigmentation and Eyelid Rash Treatment in Katy and Houston, Texas
At Village Dermatology, we specialize in:
Post-inflammatory hyperpigmentation treatment
Eyelid dermatitis management
Facial discoloration
Allergy-related skin conditions
Medical dermatology for adults
If you are experiencing dark patches, eyelid rash, or uneven skin tone in Katy, Texas or Houston, Texas, our dermatology team is here to help.
Schedule your consultation today and restore clarity and confidence to your skin.
Why Did I Suddenly Break Out in an Itchy Rash on My Face?
A 74-year-old woman presented to Village Dermatology in Katy, Texas with a sudden itchy facial rash diagnosed as allergic contact dermatitis. Learn how expert dermatologic care in Houston and Katy can help treat and prevent facial rashes.
At Village Dermatology in Katy, Texas and Houston, Texas, we frequently see patients who are alarmed by sudden facial rashes. A 74-year-old female recently came to our office as a new patient with a one-week history of a severely itchy facial rash.
Her main concern was simple and urgent:
“Why did I suddenly break out in an itchy rash on my face?”
Here’s what we discovered — and how we helped.
Sudden Facial Rash in a 74-Year-Old Woman
The patient reported:
Sudden onset of itching on the face
Moderate severity
Rash present for one week
Severe pruritus (itching) at its peak
Recent treatment with oral prednisone
Use of over-the-counter Benadryl cream
Using dermoscopic evaluation and reviewing submitted photographs taken during the peak of the eruption, the clinical findings were most consistent with:
Allergic Contact Dermatitis (ACD)
What Is Allergic Contact Dermatitis?
Allergic contact dermatitis is a delayed hypersensitivity reaction that occurs when the skin comes into contact with a substance that triggers an immune response.
Common triggers include:
New skincare products
Fragrances
Cosmetics
Hair dyes
Nail products
Sunscreens
Metals (nickel)
Plants
Scented soaps
Sometimes the reaction appears days after exposure, making it difficult to identify the culprit.
Why Patch Testing Was Delayed
Because the patient was currently taking oral prednisone, we advised that patch testing must be postponed for at least three weeks.
Steroids can suppress immune responses and cause false-negative patch testing results.
In the meantime, we began insurance verification so testing can be scheduled promptly once she is eligible.
Patch testing is often critical when:
The rash persists
The trigger is unclear
Multiple potential allergens are involved
Treatment Plan for Allergic Contact Dermatitis
At Village Dermatology in Katy and Houston, we focus on both immediate relief and long-term prevention.
Immediate Treatment
Apply twice daily for two weeks
Then use as needed for flares
Topical steroids help calm inflammation and reduce itching.
Essential Skincare Reset
We advised the patient to:
Discontinue all current skincare products
Avoid fragrances and scented products
Use only hypoallergenic, unscented soaps
Avoid new cosmetics, shampoos, and sunscreens
Use gentle moisturizers
When allergic contact dermatitis occurs, simplifying your skincare routine is crucial.
Additional Finding: Facial Ecchymosis from CPAP Mask
During examination, we also noted non-palpable purpuric patches (bruising) on both cheeks.
These findings were consistent with:
Ecchymosis (Bruising)
In this case, likely caused by pressure from the patient’s CPAP mask.
Patients using CPAP devices may develop:
Pressure-related bruising
Skin fragility
Friction-related irritation
We recommended:
Loosening or refitting the CPAP mask
Applying a barrier cream such as Desitin to reduce friction
Monitoring for worsening bruising
Most ecchymoses resolve within 3–4 weeks without treatment.
When Should You See a Dermatologist for a Facial Rash?
Seek evaluation if:
A rash appears suddenly without explanation
Itching is severe
Over-the-counter treatments are not helping
The rash spreads or worsens
You suspect a product reaction
Facial skin is delicate, and misdiagnosis can prolong symptoms.
Early dermatologic evaluation helps prevent chronic inflammation and skin damage.
Expert Rash Treatment in Katy and Houston, Texas
At Village Dermatology, we specialize in diagnosing and treating:
Allergic contact dermatitis
Facial rashes
Itchy skin conditions
CPAP-related skin irritation
Chronic inflammatory skin disorders
If you are experiencing a sudden facial rash in Katy, Texas or Houston, Texas, our board-certified dermatology team is here to help.
Schedule your consultation today and let us help restore your skin’s health and comfort.
Why Is My Face So Red, Flaky, and Itchy — and Why Won’t It Go Away?
An 80-year-old male presented to Village Dermatology in Katy, Texas with a chronic red, flaky facial rash diagnosed as seborrheic dermatitis. Learn how expert dermatologic care in Houston and Katy can effectively manage persistent facial rashes.
At Village Dermatology in Katy, Texas and Houston, Texas, we frequently see patients who are frustrated by persistent facial rashes. Recently, an 80-year-old gentleman came to our office with concerns about a red, itchy, flaking rash on his face that had been present for several months.
He asked a question we hear often:
“Why is my face so red, flaky, and itchy — and why won’t it go away?”
Let’s break down what was happening and how we helped.
Understanding Chronic Facial Rashes in Older Adults
This patient reported:
Persistent redness on the forehead
Flaking and scaling skin
Itching and irritation
Symptoms lasting for months
On examination using dermoscopy, we noted pink-to-orange scaly plaques distributed across:
The right inferior forehead
The left inferior forehead
The posterior mid-parietal scalp
Based on the clinical presentation, the diagnosis was seborrheic dermatitis.
What Is Seborrheic Dermatitis?
Seborrheic dermatitis is a chronic inflammatory skin condition that commonly affects:
Face (especially eyebrows, forehead, sides of nose)
Scalp
Ears
Beard area
It presents with:
Redness
Flaking
Greasy or dry scale
Itching
It is extremely common in older adults and can flare due to:
Stress
Illness
Changes in environment
Underlying medical conditions
Many patients in assisted living or transitional care facilities experience flares due to environmental changes and stress on the body.
The important thing to understand is:
Seborrheic dermatitis is chronic. It has periods of flares and remissions. It can be controlled, but not permanently cured.
Treatment Plan for Facial Seborrheic Dermatitis
At Village Dermatology in Katy and Houston, we focus on creating simple, practical treatment regimens that are easy to follow.
For this patient, we recommended:
1. Medicated Shampoo
Ketoconazole 2% shampoo
Use 2–3 times per week during flares
Leave on for 5–10 minutes before rinsing
Use once weekly for maintenance
This helps reduce yeast overgrowth that contributes to inflammation.
2. Combination Topical Therapy for Flares
During flare-ups:
Mix ketoconazole cream with hydrocortisone 2.5% cream
Apply to affected areas on the face and neck twice daily
Use for 2 weeks only during flares
We carefully counsel patients that prolonged steroid use on the face can cause:
Skin thinning
Lightening of the skin
Visible small blood vessels
Using low-potency steroids appropriately and only during flares minimizes these risks.
3. Gentle Skin Care Routine
We advised:
Dove Sensitive Skin body wash
Daily moisturizing with CeraVe or Vanicream
Avoid harsh soaps or scrubs
Gentle skincare is essential for managing seborrheic dermatitis long term.
Additional Concerns Addressed During the Visit
Onychomycosis (Toenail Fungus)
The patient had longstanding toenail fungus. We discussed that treatment is optional if it is not bothersome.
Key counseling points:
Oral medications are more effective but carry potential side effects.
Topical treatments (like OTC Lamisil) may help if fungus spreads to surrounding skin.
Lower Extremity Ulcers
The patient also had ulcers on the right great toe and left ankle following surgery. Because he has diabetes and neuropathy, we emphasized:
Close wound care follow-up
Monitoring for infection
Continued coordination with wound care specialists
Fortunately, there were no signs of infection during the visit.
When Should You See a Dermatologist for a Facial Rash?
You should schedule an evaluation if:
The rash lasts more than a few weeks
Over-the-counter products are not helping
The rash spreads
There is significant itching or discomfort
You are unsure of the diagnosis
Many patients assume persistent facial redness is just “dry skin.” In reality, it may be seborrheic dermatitis, rosacea, psoriasis, or another inflammatory condition.
An accurate diagnosis makes all the difference.
Expert Seborrheic Dermatitis Care in Katy and Houston, Texas
At Village Dermatology, we specialize in diagnosing and managing chronic skin conditions in patients of all ages — including elderly patients in transitional care and assisted living facilities.
If you or a loved one is experiencing:
Red, flaky facial skin
Chronic scalp scaling
Persistent itching
Recurrent facial rashes
We are here to help.
Schedule an appointment at Village Dermatology in Katy, Texas or Houston, Texas today.
Clearer, healthier skin is possible — even with chronic conditions.
Melasma Treatment Follow-Up in Katy & Houston, TX: Case Report of Persistent Facial Hyperpigmentation
A 50-year-old male followed up for melasma treatment with tretinoin and oral tranexamic acid. Learn how Village Dermatology in Katy and Houston, Texas manages persistent facial hyperpigmentation.
By: Dr. Caroline Vaughn
Melasma can be one of the most frustrating pigment conditions to treat due to its chronic, relapsing nature. At Village Dermatology, we take a multimodal and maintenance-based approach to help patients achieve long-term improvement. This case highlights a melasma follow-up visit in a 50-year-old male treated in Katy and Houston, Texas.
Patient Presentation
A 50-year-old male returned for a three-month follow-up for melasma affecting the left central malar cheek.
At his previous visit (August 27, 2025), he was prescribed:
Tretinoin 0.025% cream (pea-sized amount, 2–3 nights weekly increasing to nightly as tolerated)
Oral tranexamic acid 650 mg, ½ tablet twice daily
Despite adherence to treatment, the patient reported minimal improvement. He noted that a prior compounded hydroquinone formulation had provided slightly better results.
Clinical Examination
A focused facial examination was performed using dermoscopy.
Findings included:
Ill-defined hyperpigmented patches
Periorbital/malar distribution
Located primarily on the left central malar cheek
Overall, the melasma appeared relatively controlled but with persistent residual pigmentation.
Diagnosis
Melasma
Chronic hyperpigmentation disorder affecting sun-exposed facial areas.
Treatment Plan
After extensive discussion, the following plan was agreed upon:
Restart Compounded Hydroquinone
Resume a 3-month course
Emphasized that hydroquinone is not intended for long-term continuous use
Reviewed risks including rare pseudoochronosis
Continue Tretinoin 0.025%
Safe for long-term maintenance therapy
Apply pea-sized amount nightly as tolerated
Procedural Options Discussed
Melanage® peel
Superficial chemical peels
Other pigment-targeting treatments
The patient may consider a Melanage peel in the future.
Importance of Sun Protection
Strict daily photoprotection was emphasized as the foundation of melasma management:
Reapplication during sun exposure
Sun avoidance when possible
Protective hats and clothing
Without consistent sun protection, melasma recurrence is common.
Patient Counseling & Education
Expectations
Melasma is chronic and often triggered by:
Sun exposure
Hormonal changes
Heat
Maintenance therapy is typically required
Retinoid Counseling
Apply at bedtime
Wait 30 minutes after washing face
Use moisturizer if dryness occurs
When to Contact the Office
If melasma worsens
If medication side effects develop
If pigment changes appear concerning
Clinical photos were obtained for monitoring progress. The patient will message the office if he needs a refill on compounded hydroquinone.
Follow-Up
Follow up in 4 months for reassessment
Long-term maintenance visit annually
Advanced Melasma Treatment in Katy & Houston
At Village Dermatology, we provide comprehensive melasma management including:
Topical retinoids
Hydroquinone therapy
Oral tranexamic acid
Chemical peels
Laser treatments
If you are struggling with facial hyperpigmentation or dark patches, our dermatology team in Katy and Houston, Texas can help create a customized treatment plan.
Sebaceous Hyperplasia Treatment Case Report: Cosmetic Lesion Removal in Katy & Houston, TX
A 22-year-old male underwent cosmetic electrodesiccation for sebaceous hyperplasia on the nose and cheeks. Learn how Village Dermatology in Katy and Houston, Texas treats benign facial lesions safely and effectively.
By: Dr. Ashley Baldree
Facial skin lesions that darken or enlarge can understandably cause concern, especially in young adults. At Village Dermatology, we carefully evaluate all changing facial lesions to rule out concerning pathology and provide safe, effective cosmetic treatment options. This case highlights the diagnosis and cosmetic removal of sebaceous hyperplasia in a 22-year-old patient in Katy and Houston, Texas.
Patient Presentation
A 22-year-old male, an established patient, presented for evaluation of multiple facial skin lesions located on:
Nose
Right cheek
Left cheek
The lesions had been present for several months and were described as:
Darkening
Enlarging
Irregular in appearance
Moderate in severity
The lesions had not been previously treated. The patient requested evaluation and management.
Clinical Examination
A focused dermatologic examination of the scalp, head, and face was performed.
Findings revealed multiple small papules distributed on:
Nasal dorsum
Right nasal sidewall
Nasal tip and supratip
Left superior medial malar cheek
Left medial malar cheek
The appearance was consistent with sebaceous hyperplasia, a benign enlargement of oil glands.
Diagnosis
Sebaceous Hyperplasia
Benign enlarged sebaceous (oil) glands of the face.
Treatment Plan
The benign nature of sebaceous hyperplasia was reviewed with the patient. Treatment options were discussed, including:
Electrodessication
Laser therapy
The patient elected to proceed with cosmetic electrodesiccation.
Procedure Details
10 lesions treated
Locations: nasal dorsum, bilateral malar cheeks, nasal sidewall, tip, and supratip
Informed consent obtained
Risks reviewed, including:
Crusting
Scabbing
Blistering
Pigment changes
Recurrence
Infection
Scarring
Detailed post-procedure care instructions were provided.
Post-Procedure Instructions
Apply Vaseline to treated areas if crusting occurs
Avoid picking or scratching
Use daily sun protection (SPF 30+)
Expect mild redness and scabbing during healing
Patients were instructed to contact the office if lesions fail to improve or if signs of infection develop.
Additional Cosmetic Consultation
The patient also consulted regarding acne scarring, with plans to consider treatment after completion of his isotretinoin (Accutane®) course.
Potential future treatments discussed included:
CO₂ laser resurfacing
Subcision
Chemical peels
Cosmetic Dermatology in Katy & Houston
Sebaceous hyperplasia is common in young adults and can mimic more concerning lesions. At Village Dermatology, we provide expert facial lesion evaluation and advanced cosmetic treatments, including electrodesiccation and laser therapy, in Katy and Houston, Texas.
If you notice enlarging or changing facial lesions, schedule a professional evaluation for peace of mind.
Plantar Callus Treatment Case Report: Managing Hyperkeratotic Foot Lesions in Katy & Houston, TX
A 38-year-old male was evaluated for plantar calluses on the foot. Learn how Village Dermatology in Katy and Houston, Texas treats hyperkeratotic foot lesions using urea 40% and keratolytic therapy.
By: Dr. Ashely Baldree
Thickened skin on the soles of the feet is a common concern, especially in active adults. At Village Dermatology, we frequently evaluate lesions on the plantar surface to determine whether they represent benign calluses, warts, or more concerning growths. This case highlights the evaluation and treatment of plantar calluses in a patient seen in Katy and Houston, Texas.
Patient Presentation
A 38-year-old male presented as a new patient for evaluation of a skin lesion on the right plantar surface of the foot. The lesion had been present for several months and was:
Asymptomatic
Stable in size
Not previously treated
Not associated with a family history of melanoma
The patient requested evaluation to ensure the lesion was benign and to discuss treatment options.
Clinical Examination
A focused dermatologic examination of both feet was performed using dermoscopy.
Findings included:
Hyperkeratotic plaques
Located on pressure-bearing areas:
Right medial plantar midfoot
Left medial plantar heel
The appearance and distribution were consistent with plantar calluses caused by friction and pressure rather than a neoplastic process.
Assessment
Callus
Hyperkeratotic plaques on pressure-bearing surfaces of the feet.
Treatment Plan
The patient was reassured that the lesions were benign calluses resulting from chronic friction.
Recommended Treatment:
Urea 40% topical cream, applied nightly to the soles
Samples of urea lotion provided in-office
Continue use of keratolytic agents such as:
Amlactin®
Duofilm®
Mediplast®
Urea 40% helps soften and break down thickened skin, improving texture and comfort over time.
Patient Counseling & Education
Why Calluses Form
Calluses develop due to:
Repeated friction
Pressure from footwear
Abnormal weight distribution
Expectations
Improvement typically occurs with consistent keratolytic therapy
Reduction of friction (proper footwear, insoles) is key to prevention
Calluses may recur if pressure persists
When to Contact the Office
If lesions worsen
If pain develops
If no improvement after several months of treatment
Follow-Up
Follow up as needed if symptoms worsen or fail to improve.
Expert Foot & Skin Care in Katy & Houston
At Village Dermatology, we evaluate all plantar lesions carefully to rule out warts, atypical growths, or precancerous changes. Whether you're dealing with calluses, dry cracked heels, plantar warts, or other foot skin conditions, our dermatology team provides personalized, evidence-based treatment.
If you have thickened or persistent skin lesions on your feet, schedule an evaluation with Village Dermatology in Katy or Houston, Texas.