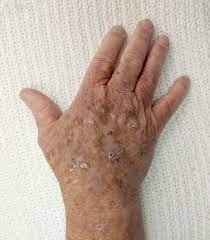
Actinic Keratosis
What is an actinic keratosis?
An actinic keratosis (AK) is a precancerous skin growth that appears on areas of the skin that have received chronic sun exposure. They appear as small rough spots on the skin that can range in size from the size of a pencil point to the size of a quarter. They are usually pink to red in color; however, they can also appear yellowish, brownish, or whitish. Often you may feel these spots before you see them, and they are often surrounded by evidence of sun damage, including enlarged blood vessels and wrinkling or yellowing of the skin. Eventually actinic keratoses become rougher and more crusted, and they can become sore or painful to the touch. A cutaneous horn is a special type of actinic keratosis which protrudes from the skin in a thick, horn-like manner. Actinic cheilitis refers to precancerous damage of the lip, and it appears as a rough, scaling spot on the lower lip.
CAUSES
People who are fair-skinned an who have spent a good deal of time outdoors are the most at risk for actinic keratoses, though they can also develop in people with darker skin types. In addition, people who work outdoors or who have exposed their skin to indoor tanning are also at risk. With time and long-term sun exposure, the skin takes on a wrinkled, sallow, mottled appearance, and, eventually, precancerous lesions develop. Other populations at risk include people with suppressed immune systems, such as transplant patients, as well as patients with psoriasis or eczema who have been treated with phototherapy. Such individuals should be screened annually for evidence of actinic damage, and they should follow sun safety measures at all times.
The most common areas for actinic keratoses are those that have received chronic sun exposure, including the face, particularly the cheeks and nose, scalp, back of the neck, upper chest, and the backs of the hands and forearms. In addition, men are more likely than women to develop actinic keratoses on the tops of the ears, because the longer hairstyles of women tend to protect those areas.
TREATMENT OF ACTINIC KERATOSES
A pre-cancer is just what the name implies: it is not yet a cancer, but if left untreated, it may develop into a skin cancer. In truth, only a small percentage of actinic keratoses (AKs) may go on to develop into actual skin cancers, and the process may take years. However, if left alone, they may develop into squamous cell carcinomas that do have a small potential for spread through the body. Early detection and treatment of AKs can prevent this from happening, and it can keep you from having to undergo a more invasive procedure. A board-certified dermatologist can diagnose actinic keratoses simply by looking at your skin. If needed, a skin biopsy can be done to confirm the diagnosis; however, this is typically not necessary.
Fortunately, treatment of actinic keratoses is relatively straightforward. The doctors at Village Dermatology may discuss the following options with you:
Cryosurgery: Freezing an actinic keratosis with liquid nitrogen can cause the lesion to slough off and disappear. This is a relatively easy, quick procedure with little downtime, and it is the most common method of treatment; however the treated spots may appear red for about a week or two.
Surgical removal: If hypertrophic (relatively large and raised off the skin), your doctor may elect to remove the actinic keratosis via shave biopsy. This is done commonly for cutaneous horns.
Topical 5-fluorouracil (5-FU, Efudex, Carac): These medications are cream versions of a chemotherapy medication. Creams containing this ingredient cause the actinic keratoses to become red and inflamed before they fall off. The treatment is quite effective; however, during treatment, the medication can produce an uncomfortable and unsightly appearance to the skin, making it difficult for some patients to tolerate. It is good for areas that have a large amount of sun damage and many actinic keratoses to help make the skin much smoother and even-toned with fewer precancerous lesions.
Topical imiquimod (Aldara, Zyclara): These medications are immune stimulators that have similar indications and outcomes as topical 5-FU.
Topical diclofenac (Solaraze): This gel is a topical non-steroidal anti-inflammatory drug that is much gentler than 5-FU and imiquimod. However, it must be applied twice daily for a much longer interval (as long as 2-3 months) to have the same effect.
Topical ingenol mebutate (Picato): This is a plant-derived substance that induces cell death. Its advantage is that dosing is very rapid, with topical application over 2-3 days. A very brisk inflammatory response is typically seen, but treatment is complete by about 10 days.
Photodynamic therapy (PDT): This treatment involved pretreating the skin with a dye (aminolevulinic acid) that sensitizes the skin to light. The dye is left on for 1-2 hours, and the skin is then treated with a laser or other light source that activates the dye and treats the precancers. It works best for patients with many AKs, particularly because of the amount of time involved with the procedure. Patients often need to avoid sun exposure or exposure to intense fluorescent light for two days following the treatments.
Fraxel: Fraxel is a non-ablative laser used for the treatment of actinic keratoses. The 1927 thulium fiber laser allows resurfacing of the skin with only a few days of downtime. The procedure is quick and effective, with an approximately 85% reduction in the number of lesions. Insurance typically does not cover this procedure. http://www.jaad.org/article/S0190-9622%2812%2900635-4/abstract
Really, as is the case for many diseases, prevention is the best treatment. While you can’t undo the UV exposure that you’ve already gotten, you can definitely keep your skin from getting any worse. It’s important to follow sun safety measures on a regular basis and to start right away.
If you think you have an actinic keratosis or other suspicious lesion, it is best to contact us to make an appointment for evaluation. complaints account for a large number of visits to the doctor's office. Dermatologists treat a variety of skin conditions, and their training gives them the unique expertise to diagnose and treat almost anything that may be bothering you. Below are some of the more common things we see:
LIQUID NITROGEN POST TREATMENT CARE
Click here for a printable PDF of these instructions.
Cryotherapy using liquid nitrogen is used to treat skin lesions such as warts, seborrheic keratoses (age spots), brown spots/freckles, and actinic keratoses (precancers) among other things.
Following treatment with liquid nitrogen, you may notice pain, throbbing, and immediate redness and swelling around the treated area. At the time, swelling may become so intense that a blister forms at the site of the freezing treatment. Rarely, a blood blister may form, but will dry up and scab within a few days. This is a normal part of the healing process and the scab will fall off or heal within 1-2 weeks. The skin might be discolored at the treatment site, but normal color will return within 1-2 months. Cryotherapy does not cause scarring.
Wound Care Instructions
1. There are no restrictions in your daily activities such as washing your face/hands, bathing or showering.
2. Take Tylenol for any discomfort or pain.
3. You may apply an ointment (such as Vaseline) to the area twice a day as needed.
4. Protect the wound from the sun.
5. If a blister forms that is uncomfortable, you can sterilize a needle with rubbing alcohol and pierce the side of the blister, allowing the fluid to drain out. Allow the roof of the blister to collapse onto the wound to act as a natural Band-Aid.
6. If a precancerous spot was treated, please let us know immediately if the spot fails to resolve before your next appointment. If it does not respond to the treatment, you must return to the clinic in order to reevaluate.
If you have any questions regarding this treatment, please feel free to call us at 713.952.8400.